Nutrient, Fibre, and FODMAP Intakes and Food-related Quality of Life in Patients with Inflammatory Bowel Disease, and Their Relationship with Gastrointestinal Symptoms of Differing Aetiologies
- PMID: 34216206
- PMCID: PMC8684455
- DOI: 10.1093/ecco-jcc/jjab116
Nutrient, Fibre, and FODMAP Intakes and Food-related Quality of Life in Patients with Inflammatory Bowel Disease, and Their Relationship with Gastrointestinal Symptoms of Differing Aetiologies
Abstract
Background and aims: Certain foods are reported as gut symptom triggers in inflammatory bowel disease [IBD], and fructans are shown to worsen non-inflammatory symptoms in inactive IBD, which may result in self-imposed dietary restrictions. The aim of this study was to investigate nutrient and FODMAP intakes, and the relationship between gut symptoms and dietary intake, in IBD.
Methods: Nutrient, fibre, and FODMAP intakes were estimated using 7-day food records in patients with active IBD [Active IBD], inactive IBD with non-inflammatory gut symptoms [Inactive IBD-GI], inactive IBD without gut symptoms [Inactive IBD], and healthy controls. Nutrient intakes, numbers of participants achieving national recommendations, and food-related quality of life [FR-QoL] were compared across study groups.
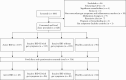
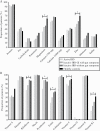
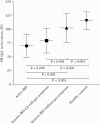
Results: Food diaries were obtained from 232 patients with IBD [65 Active IBD, 86 Inactive IBD-GI, 81 Inactive IBD] and 84 healthy controls. Patients with Active IBD had significantly lower intakes of numerous micronutrients, including iron, folate, and vitamin C, compared with controls. All IBD groups consumed less total fibre [4.5 to 5.8 g/day] than controls [p = 0.001], and total FODMAP and fructan intakes were lower in Active IBD compared with controls. Strikingly, FR-QoL was significantly lower in all IBD groups compared with controls [all p = 0.001].
Conclusions: This study revealed lower intakes of fibre, FODMAPs, and micronutrients, in addition to poorer FR-QoL, in Active IBD and Inactive IBD-GI with gut symptoms compared with healthy controls. Future research should address dietary restrictions responsible for these differences.
Keywords: FR-QoL; Inflammatory bowel disease; diet; food-related quality of life; nutrition.
© The Author(s) 2021. Published by Oxford University Press on behalf of European Crohn’s and Colitis Organisation.
Figures
References
-
- Prince A, Whelan K, Moosa A, Lomer MC, Reidlinger DP. Nutritional problems in inflammatory bowel disease: the patient perspective. J Crohns Colitis 2011;5:443–50. - PubMed
-
- Czuber-Dochan W, Morgan M, Hughes LD, Lomer MCE, Lindsay JO, Whelan K. Perceptions and psychosocial impact of food, nutrition, eating and drinking in people with inflammatory bowel disease: a qualitative investigation of food-related quality of life. J Hum Nutr Diet 2020;33:115–27. - PubMed
-
- Whelan K, Murrells T, Morgan M, et al. . Food-related quality of life is impaired in inflammatory bowel disease and associated with reduced intake of key nutrients. Am J Clin Nutr 2021;113:832–44. - PubMed
-
- Lomer MC, Hart AL, Verjee A, Daly A, Solomon J, Mclaughlin J. What are the dietary treatment research priorities for inflammatory bowel disease? A short report based on a priority setting partnership with the James Lind Alliance. J Hum Nutr Diet 2017;30:709–13. - PubMed
-
- Mijac DD, Janković GL, Jorga J, Krstić MN. Nutritional status in patients with active inflammatory bowel disease: prevalence of malnutrition and methods for routine nutritional assessment. Eur J Intern Med 2010;21:315–9. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

