Cataract Surgery with or without Intraocular Lens Implantation in Pediatric Uveitis: A Systematic Review with Meta-Analyses
- PMID: 34221492
- PMCID: PMC8213487
- DOI: 10.1155/2021/5481609
Cataract Surgery with or without Intraocular Lens Implantation in Pediatric Uveitis: A Systematic Review with Meta-Analyses
Abstract
Purpose: To systematically review the results of comparative studies of modern cataract surgery in pediatric uveitis with or without intraocular lens (IOL) implantation and to perform comparative meta-analyses to compare visual acuity outcomes and complication rates.
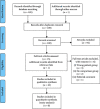
Methods: On 12 November 2020, we systematically searched the Cochrane Central, PubMed/MEDLINE, EMBASE, ClinicalTrials.gov, and all affiliated databases of the Web of Science. Two authors independently reviewed studies and extracted data. Studies were reviewed qualitatively in text and quantitatively with meta-analyses. Outcome measures were preoperative and postoperative best-corrected visual acuity (BCVA), inflammation control, and rates of postoperative complications.
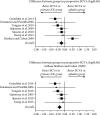
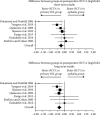
Results: Ten studies of 288 eyes were eligible for review of which the majority were eyes with juvenile idiopathic arthritis-associated uveitis. Summary estimates revealed that the BCVA was better in pseudophakic eyes vs. aphakic eyes (1-year postoperative: -0.23 logMAR, 95% CI: -0.43 to -0.03 logMAR, P=0.027; 5-year postoperative: -0.35 logMAR, 95% CI: -0.51 to -0.18 logMAR, P=0.000036). Pseudophakic eyes had more visual axis opacification (OR 6.76, 95% CI: 2.73 to 16.8, P=0.000036) and less hypotony (OR 0.19, 95% CI: 0.04 to 0.95, P=0.044).
Conclusions: In modern era cataract surgery on eyes with pediatric uveitis with IOL implantation leads to satisfactory and superior visual outcomes and no differences in complication rates apart from an increased prevalence of visual axis opacification and a decreased prevalence of hypotony when compared to aphakia. However, limitations of the retrospective design and the presence of selection bias necessitate a careful interpretation.
Copyright © 2021 Diana Chabané Schmidt et al.
Conflict of interest statement
The authors declare that they have no conflicts of interest.
Figures

Similar articles
-
Cataract surgery in children with chronic uveitis.Ophthalmology. 2000 Jul;107(7):1255-60. doi: 10.1016/s0161-6420(00)00160-3. Ophthalmology. 2000. PMID: 10889094
-
Long-term outcomes of cataract surgery in children with uveitis.Indian J Ophthalmol. 2019 Apr;67(4):490-495. doi: 10.4103/ijo.IJO_846_18. Indian J Ophthalmol. 2019. PMID: 30900580 Free PMC article.
-
Long-term ocular complications in aphakic versus pseudophakic eyes of children with juvenile idiopathic arthritis-associated uveitis.Br J Ophthalmol. 2010 Sep;94(9):1145-9. doi: 10.1136/bjo.2009.167379. Epub 2010 Jun 16. Br J Ophthalmol. 2010. PMID: 20558424
-
[Studies on clinical pathophysiology of pseudophakic/aphakic eyes--a journey of 4 decades].Nippon Ganka Gakkai Zasshi. 2008 Mar;112(3):214-45; discussion 246. Nippon Ganka Gakkai Zasshi. 2008. PMID: 18411712 Review. Japanese.
-
Efficacy and safety of vitrectomy for congenital cataract surgery: a systematic review and meta-analysis based on randomized and controlled trials.Acta Ophthalmol. 2019 May;97(3):233-239. doi: 10.1111/aos.13974. Epub 2018 Nov 22. Acta Ophthalmol. 2019. PMID: 30565873 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources

