Financial burden of postoperative complications following colonic resection: A systematic review
- PMID: 34232193
- PMCID: PMC8270623
- DOI: 10.1097/MD.0000000000026546
Financial burden of postoperative complications following colonic resection: A systematic review
Abstract
Background: Colonic resection is a common surgical procedure that is associated with a high rate of postoperative complications. Postoperative complications are expected to be major contributors to hospital costs. Therefore, this systematic review aims to outline the health costs of postoperative complications following colon resection surgery.
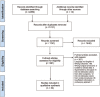
Methods: MEDLINE, Excerpta Medica database, Cochrane, and Economics literature medical databases were searched from 2010 to 2019 to identify English studies containing an economic evaluation of postoperative complications following colonic resection in adult patients. All surgical techniques and indications for colon resection were included. Eligible study designs included randomized trials, comparative observational studies, and conference abstracts.
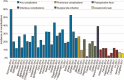
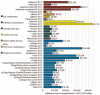
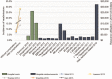
Results: Thirty-four articles met the eligibility criteria. We found a high overall complication incidence with associated increased costs ranging from $2290 to $43,146. Surgical site infections and anastomotic leak were shown to be associated with greater resource utilization relative to other postoperative complications. Postoperative complications were associated with greater incidence of hospital readmission, which in turn is highlighted as a significant financial burden. Weak evidence demonstrates increased complication incidence and costlier complications with open colon surgery as compared to laparoscopic surgery. Notably, we identified a vast degree of heterogeneity in study design, complication reporting and costing methodology preventing quantitative analysis of cost results.
Conclusions: Postoperative complications in colonic resection appear to be associated with a significant financial burden. Therefore, large, prospective, cost-benefit clinical trials investigating preventative strategies, with detailed and consistent methodology and reporting standards, are required to improve patient outcomes and the cost-effectiveness of our health care systems.
Copyright © 2021 the Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
The authors have no funding and conflicts of interest to disclose.
Figures
References
-
- Xu K, Soucat A, Kutzin J, et al. . Public Spending on Health: A Closer Look at Global Trends. Geneva: World Health Organization; 2018 (WHO/HIS/HGF/HFWorkingPaper/18.3). Licence: CC BY-NC-SA 3.0 IGO. Available from: http://www.who.int/iris/handle/10665/276728. Accessed April 6, 2019
-
- Vonlanthen R, Slankamenac K, Breitenstein S, et al. . The impact of complications on costs of major surgical procedures: a cost analysis of 1200 patients. Ann Surg 2011;254:907–13. - PubMed
-
- Patel AS, Bergman A, Moore BW, et al. . The economic burden of complications occurring in major surgical procedures: a systematic review. Appl Health Econ Health Policy 2013;11:577–92. - PubMed
-
- Schilling PL, Dimick JB, Birkmeyer JD. Prioritizing quality improvement in general surgery. J Am Coll Surg 2008;207:698–704. - PubMed
-
- de Silva S, Ma C, Proulx MC, et al. . Postoperative complications and mortality following colectomy for ulcerative colitis. Clin Gastroenterol Hepatol 2011;9:972–80. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

