Standard prophylactic versus intermediate dose enoxaparin in adults with severe COVID-19: A multi-center, open-label, randomized controlled trial
- PMID: 34236768
- PMCID: PMC8420176
- DOI: 10.1111/jth.15450
Standard prophylactic versus intermediate dose enoxaparin in adults with severe COVID-19: A multi-center, open-label, randomized controlled trial
Abstract
Background: Coronavirus disease 2019 (COVID-19) is associated with coagulopathy but the optimal prophylactic anticoagulation therapy remains uncertain and may depend on COVID-19 severity.
Objective: To compare outcomes in hospitalized adults with severe COVID-19 treated with standard prophylactic versus intermediate dose enoxaparin.
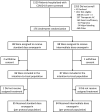
Methods: We conducted a multi-center, open-label, randomized controlled trial comparing standard prophylactic dose versus intermediate dose enoxaparin in adults who were hospitalized with COVID-19 and admitted to an intensive care unit (ICU) and/or had laboratory evidence of coagulopathy. Patients were randomly assigned in a 1:1 ratio to receive standard prophylactic dose enoxaparin or intermediate weight-adjusted dose enoxaparin. The primary outcome was all-cause mortality at 30 days. Secondary outcomes included arterial or venous thromboembolism and major bleeding.
Results: A total of 176 patients (99 males and 77 females) underwent randomization. In the intention-to-treat population, all-cause mortality at 30 days was 15% for intermediate dose enoxaparin and 21% for standard prophylactic dose enoxaparin (odds ratio, 0.66; 95% confidence interval, 0.30-1.45; P = .31 by Chi-square test). Unadjusted Cox proportional hazards modeling demonstrated no significant difference in mortality between intermediate and standard dose enoxaparin (hazard ratio, 0.67; 95% confidence interval, 0.33-1.37; P = .28). Arterial or venous thrombosis occurred in 13% of patients assigned to intermediate dose enoxaparin and 9% of patients assigned to standard dose enoxaparin. Major bleeding occurred in 2% of patients in each arm.
Conclusion: In hospitalized adults with severe COVID-19, standard prophylactic dose and intermediate dose enoxaparin did not differ significantly in preventing death or thrombosis at 30 days.
Keywords: COVID-19 disease; anticoagulant; blood coagulation; enoxaparin; thrombosis.
© 2021 International Society on Thrombosis and Haemostasis.
Figures

References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

