A case of hepatic splenosis in the setting of iron overload; multimodal and literature review
- PMID: 34257788
- PMCID: PMC8259227
- DOI: 10.1016/j.radcr.2021.05.037
A case of hepatic splenosis in the setting of iron overload; multimodal and literature review
Abstract
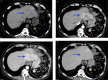
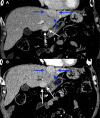
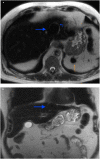
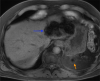
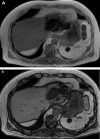
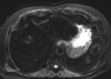
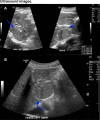
Hepatic splenosis, a rare entity, is the ectopic implantation of splenic tissue into the hepatic parenchyma, most often incidentally seen in patients with a history of splenic trauma and splenectomy. We present a unique case of hepatic splenosis in a patient with hemosiderosis and splenectomy following the incidental finding of hepatic masses on pretransplant imaging. Final diagnosis was made based on cross-sectional imaging characteristics matching that of the left upper quadrant splenules alone. We discuss common characteristics of hepatic splenosis on multiple modalities, the effect of iron deposition on the imaging characteristics of hepatic and splenic tissue and how that impacts the differential and diagnosis. This case highlights the unique imaging characteristics hepatic splenosis can have particularly in the setting of hemosiderosis. Hepatic splenosis imaging diagnosis has a significant advantage over tissue diagnosis in terms of decreased risk, time and cost.
Keywords: CT, Computed Tomography; ESRD, End Stage Renal Disease; HS, Hepatic Splenosis; Hemosiderosis; Hepatic masses; Hepatic splenosis; Iron deposition; Iron overload; MRI, Magnetic Resonance Imaging; Siderosis; Splenectomy; Splenosis; Tc-99m-DRBC, Tc-99m labelled heat-denatured red blood cells; US, Ultrasound.
© 2021 The Authors. Published by Elsevier Inc. on behalf of University of Washington.
Figures
Similar articles
-
Intrahepatic and intra-abdominal splenosis: A case report and review of literature.World J Hepatol. 2019 Dec 27;11(12):773-779. doi: 10.4254/wjh.v11.i12.773. World J Hepatol. 2019. PMID: 31966909 Free PMC article.
-
Intra-hepatic splenosis as an unexpected cause of a focal liver lesion in a patient with hepatitis C and liver cirrhosis: a case report.Cases J. 2009 Aug 19;2:8335. doi: 10.4076/1757-1626-2-8335. Cases J. 2009. PMID: 19830070 Free PMC article.
-
Intrahepatic splenosis mimicking liver cancer: report of a case and review of literature.Int J Clin Exp Pathol. 2015 Jan 1;8(1):1031-5. eCollection 2015. Int J Clin Exp Pathol. 2015. PMID: 25755814 Free PMC article. Review.
-
Hepatic splenosis: Rare yet important - A case report and literature review.J Int Med Res. 2019 Apr;47(4):1793-1801. doi: 10.1177/0300060519828901. Epub 2019 Feb 27. J Int Med Res. 2019. PMID: 30810057 Free PMC article. Review.
-
Identification of perirenal or renal splenosis from undetermined masses: case report and review of the literature.Clin Nephrol. 2014 Oct;82(4):263-7. doi: 10.5414/CN107890. Clin Nephrol. 2014. PMID: 23458175 Review.
References
-
- Vernuccio F., Dimarco M., Porrello G., Cannella R., Cusmà S., Midiri M., Brancatelli G. Abdominal splenosis and its differential diagnoses: What the radiologist needs to know. Curr Probl Diagn Radiol. Mar-Apr 2021;50(2):229–235. doi: 10.1067/j.cpradiol.2020.04.012. Epub 2020 May 19. PMID: 32540140. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

