Sedation strategy and ICU delirium: a multicentre, population-based propensity score-matched cohort study
- PMID: 34285003
- PMCID: PMC8292822
- DOI: 10.1136/bmjopen-2020-045087
Sedation strategy and ICU delirium: a multicentre, population-based propensity score-matched cohort study
Abstract
Objectives: We examined the relationship between dominant sedation strategy, risk of delirium and patient-centred outcomes in adults admitted to intensive care units (ICUs).
Design: Retrospective propensity-matched cohort study.
Setting: Mechanically ventilated adults (≥ 18 years) admitted to four Canadian hospital medical/surgical ICUs from 2014 to 2016 in Calgary, Alberta, Canada.
Participants: 2837 mechanically ventilated adults (≥ 18 years) requiring admission to a medical/surgical ICU were evaluated for the relationship between sedation strategy and delirium.
Interventions: None.
Primary and secondary outcome measures: The primary exposure was dominant sedation strategy, defined as the sedative infusion, including midazolam, propofol or fentanyl, with the longest duration before the first delirium assessment. The primary outcome was 'ever delirium' identified using the Intensive Care Delirium Screening Checklist. Secondary outcomes included mortality, length of stay (LOS), ventilation duration and days with delirium. The cohort was analysed in two propensity score (patient characteristics and therapies received) matched cohorts (propofol vs fentanyl and propofol vs midazolam).
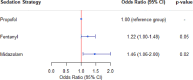
Results: 2837 patients (60.7% male; median age 57 years (IQR 43-68)) were considered for propensity matching. In propensity score-matched cohorts(propofol vs midazolam, n=712; propofol vs fentanyl, n=1732), the odds of delirium were significantly higher with midazolam (OR 1.46 (95% CI 1.06 to 2.00)) and fentanyl (OR 1.22 (95% CI 1.00 to 1.48)) compared with propofol dominant sedation strategies. Dominant sedation strategy with midazolam and fentanyl were associated with a longer duration of ventilation compared with propofol. Fentanyl was also associated with increased ICU mortality (OR 1.50, 95% CI 1.07 to 2.12)) ICU and hospital LOS compared with a propofol dominant sedation strategy.
Conclusions: We identified a novel association between fentanyl dominant sedation strategies and an increased risk of delirium, a composite outcome of delirium or death, duration of mechanical ventilation, ICU LOS and hospital LOS. Midazolam dominant sedation strategies were associated with increased delirium risk and mechanical ventilation duration.
Keywords: adult intensive & critical care; delirium & cognitive disorders; health & safety; quality in health care.
© Author(s) (or their employer(s)) 2021. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures

References
-
- Association AP . Diagnostic and Statistical Manual of Mental Disorders(DSM-5. Arlington, VA: American Psychiatric Association, 2013.
-
- Girard TD, Kress JP, Fuchs BD, et al. . Efficacy and safety of a paired sedation and ventilator weaning protocol for mechanically ventilated patients in intensive care (awakening and breathing controlled trial): a randomised controlled trial. Lancet 2008;371:126–34. 10.1016/S0140-6736(08)60105-1 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
