Glycocalyx is critical for blood-brain barrier integrity by suppressing caveolin1-dependent endothelial transcytosis following ischemic stroke
- PMID: 34286899
- PMCID: PMC8713524
- DOI: 10.1111/bpa.13006
Glycocalyx is critical for blood-brain barrier integrity by suppressing caveolin1-dependent endothelial transcytosis following ischemic stroke
Abstract
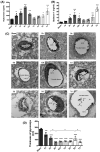
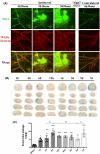
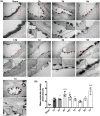
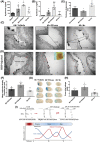
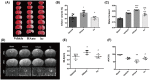
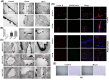
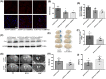
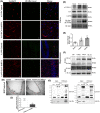
The breakdown of the blood-brain barrier (BBB) is related to the occurrence and deterioration of neurological dysfunction in ischemic stroke, which leads to the extravasation of blood-borne substances, resulting in vasogenic edema and increased mortality. However, a limited understanding of the molecular mechanisms that control the restrictive properties of the BBB hinders the manipulation of the BBB in disease and treatment. Here, we found that the glycocalyx (GCX) is a critical factor in the regulation of brain endothelial barrier integrity. First, endothelial GCX displayed a biphasic change pattern, of which the timescale matched well with the biphasic evolution of BBB permeability to tracers within the first week after t-MCAO. Moreover, GCX destruction with hyaluronidase increased BBB permeability in healthy mice and aggravated BBB leakage in transient middle cerebral artery occlusion (t-MCAO) mice. Surprisingly, ultrastructural observation showed that GCX destruction was accompanied by increased endothelial transcytosis at the ischemic BBB, while the tight junctions remained morphologically and functionally intact. Knockdown of caveolin1 (Cav1) suppressed endothelial transcytosis, leading to reduced BBB permeability, and brain edema. Lastly, a coimmunoprecipitation assay showed that GCX degradation enhanced the interaction between syndecan1 and Src by promoting the binding of phosphorylated syndecan1 to the Src SH2 domain, which led to rapid modulation of cytoskeletal proteins to promote caveolae-mediated endocytosis. Overall, these findings demonstrate that the dynamic degradation and reconstruction of GCX may account for the biphasic changes in BBB permeability in ischemic stroke, and reveal an essential role of GCX in suppressing transcellular transport in brain endothelial cells to maintain BBB integrity. Targeting GCX may provide a novel strategy for managing BBB dysfunction and central nervous system drug delivery.
Keywords: blood-brain barrier; brain edema; caveolin1; glycocalyx; ischemia stroke; transcytosis.
© 2021 The Authors. Brain Pathology published by John Wiley & Sons Ltd on behalf of International Society of Neuropathology.
Conflict of interest statement
The authors declare that they have no conflicts of interest. We confirm that we have read the Journal's position on issues involved in ethical publication and affirm that this report is consistent with those guidelines.
Figures

Similar articles
-
The Glycocalyx: The Importance of Sugar Coating the Blood-Brain Barrier.Int J Mol Sci. 2024 Aug 1;25(15):8404. doi: 10.3390/ijms25158404. Int J Mol Sci. 2024. PMID: 39125975 Free PMC article. Review.
-
Neuroinflammatory mechanisms of blood-brain barrier damage in ischemic stroke.Am J Physiol Cell Physiol. 2019 Feb 1;316(2):C135-C153. doi: 10.1152/ajpcell.00136.2018. Epub 2018 Oct 31. Am J Physiol Cell Physiol. 2019. PMID: 30379577 Free PMC article. Review.
-
Stepwise recruitment of transcellular and paracellular pathways underlies blood-brain barrier breakdown in stroke.Neuron. 2014 May 7;82(3):603-17. doi: 10.1016/j.neuron.2014.03.003. Epub 2014 Apr 17. Neuron. 2014. PMID: 24746419 Free PMC article.
-
Notoginsenoside R1 intervenes degradation and redistribution of tight junctions to ameliorate blood-brain barrier permeability by Caveolin-1/MMP2/9 pathway after acute ischemic stroke.Phytomedicine. 2021 Sep;90:153660. doi: 10.1016/j.phymed.2021.153660. Epub 2021 Jul 25. Phytomedicine. 2021. PMID: 34344565
-
Storax Inhibits Caveolae-Mediated Transcytosis at Blood-Brain Barrier After Ischemic Stroke in Rats.Front Pharmacol. 2022 Jul 8;13:876235. doi: 10.3389/fphar.2022.876235. eCollection 2022. Front Pharmacol. 2022. PMID: 35873558 Free PMC article.
Cited by
-
Flufenamic acid improves survival and neurologic outcome after successful cardiopulmonary resuscitation in mice.J Neuroinflammation. 2022 Sep 1;19(1):214. doi: 10.1186/s12974-022-02571-2. J Neuroinflammation. 2022. PMID: 36050694 Free PMC article.
-
Vascularizing the brain in vitro.iScience. 2022 Mar 17;25(4):104110. doi: 10.1016/j.isci.2022.104110. eCollection 2022 Apr 15. iScience. 2022. PMID: 35378862 Free PMC article. Review.
-
Traumatic brain injury: Bridging pathophysiological insights and precision treatment strategies.Neural Regen Res. 2026 Mar 1;21(3):887-907. doi: 10.4103/NRR.NRR-D-24-01398. Epub 2025 Mar 25. Neural Regen Res. 2026. PMID: 40145994 Free PMC article.
-
Glymphatic system in neurological disorders and implications for brain health.Front Neurol. 2025 Feb 5;16:1543725. doi: 10.3389/fneur.2025.1543725. eCollection 2025. Front Neurol. 2025. PMID: 39974364 Free PMC article. No abstract available.
-
Combining array tomography with electron tomography provides insights into leakiness of the blood-brain barrier in mouse cortex.Elife. 2024 Aug 5;12:RP90565. doi: 10.7554/eLife.90565. Elife. 2024. PMID: 39102289 Free PMC article.
References
-
- Sandoval KE, Witt KA. Blood‐brain barrier tight junction permeability and ischemic stroke. Neurobiol Dis. 2008;32(2):200–19. - PubMed
-
- Kuroiwa T, Ting P, Martinez H, Klatzo I. The biphasic opening of the blood‐brain barrier to proteins following temporary middle cerebral artery occlusion. Acta Neuropathol. 1985;68(2):122–9. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

