Mild Gestational Diabetes and Adverse Pregnancy Outcome: A Systemic Review and Meta-Analysis
- PMID: 34291067
- PMCID: PMC8286997
- DOI: 10.3389/fmed.2021.699412
Mild Gestational Diabetes and Adverse Pregnancy Outcome: A Systemic Review and Meta-Analysis
Abstract
Background and Objectives: Mild gestational diabetes (GDM) refers to the gestational hyperglycemia, which does not fulfill the diagnostic criteria for GDM. The results of studies on adverse pregnancy outcomes among women with mild GDM are controversial. Therefore, the aim of this systematic review and meta-analysis was to investigate the impact of mild GDM on the risk of adverse maternal and neonatal outcomes. Methods: A thorough literature search was performed to retrieve articles that investigated adverse maternal and neonatal outcomes in women with mild GDM in comparison with non-GDM counterparts. All populations were classified to three groups based on their diagnostic criteria for mild GDM. Heterogeneous and non-heterogeneous results were analyzed using the fixed/random effects models. Publication bias was assessed using the Harbord test. DerSimonian and Laird, and inverse variance methods were used to calculate the pooled relative risk of events. Subgroup analysis was performed based on mild GDM diagnostic criteria. Quality and risk of bias assessment were performed using standard questionnaires. Results: Seventeen studies involving 11,623 pregnant women with mild GDM and 53,057 non-GDM counterparts contributed to the meta-analysis. For adverse maternal outcomes, the results of meta-analysis showed that the women with mild GDM had a significantly higher risk of cesarean section (pooled RR: 1.3, 95% CI 1.2-1.5), pregnancy-induced hypertension (pooled RR: 1.4, 95% CI 1.1-1.7), preeclampsia (pooled RR: 1.3, 95% CI 1.1-1.5) and shoulder dystocia (pooled RR: 2.7, 95% CI 1.5-5.1) in comparison with the non-GDM population. For adverse neonatal outcomes, the pooled relative risk of macrosomia (pooled RR = 0.4, 95% CI: 1.1-1.7), large for gestational age (pooled RR = 1.7, 95% CI: 1.3-2.3), hypoglycemia (pooled RR = 1.6, 95% CI: 1.1-2.3), hyperbilirubinemia (pooled RR = 1.1, 95% CI: 1-1.3), 5 min Apgar <7 (pooled RR = 1.6, 95% CI: 1.1-2.4), admission to the neonatal intensive care unit (pooled RR = 1.5, 95% CI: 1.1-2.1), respiratory distress syndrome (pooled RR = 3.2, 95% CI: 1.8-5.5), and preterm birth (pooled RR = 1.4, 95% CI: 1.1-1.7) was significantly increased in the mild GDM women as compared with the non-GDM population. However, the adverse events of small for gestational age and neonatal death were not significantly different between the groups. Analysis of composite maternal and neonatal outcomes revealed that the risk of those adverse outcomes in the women with mild GDM in all classifications were significantly higher than the non-GDM population. Also, the meta-regression showed that the magnitude of those increased risks in both composite maternal and neonatal outcomes was similar. Conclusion: The risks of sever adverse neonatal outcomes including small for gestational age and neonatal mortality are not increased with mild GDM. However, the increased risks of most adverse maternal and neonatal outcomes are observed. The risks have similar magnitudes for all mild GDM diagnostic classifications.
Keywords: adverse maternal outcomes; adverse neonatal outcomes; diagnostic criteria; meta-analysis; mild gestational diabetes.
Copyright © 2021 Bidhendi Yarandi, Vaismoradi, Panahi, Gåre Kymre and Behboudi-Gandevani.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
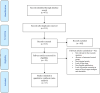
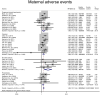




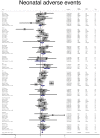
References
Publication types
LinkOut - more resources
Full Text Sources

