Evaluation of a Chronic Pain Screening Program Implemented in Primary Care
- PMID: 34313738
- PMCID: PMC8317006
- DOI: 10.1001/jamanetworkopen.2021.18495
Evaluation of a Chronic Pain Screening Program Implemented in Primary Care
Abstract
Importance: Although pain is among the most common symptoms reported by patients, primary care practitioners (PCPs) face substantial challenges identifying and assessing pain.
Objective: To evaluate a 2-step process for chronic pain screening and follow-up in primary care.
Design, setting, and participants: A cross-sectional study of patients with a primary care visit between July 2, 2018, and June 1, 2019, was conducted at a statewide, multisite federally qualified health center. Participants included 68 PCPs and 58 medical assistants from 13 sites who implemented the screening process in primary care, and 38 866 patients aged 18 years or older with a primary care visit during that time.
Exposures: Single-question assessment of pain frequency, followed by a 3-question PEG (pain, enjoyment of life, general activity) functional assessment for patients with chronic pain.
Main outcomes and measures: Adherence to a 2-step chronic pain screening and PEG process, proportion of patients with positive screening results, mean PEG pain severity greater than or equal to 7, and documented chronic painful condition diagnosis in patient's electronic health record between 1 year before and 90 days after screening.
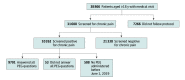
Results: Of 38 866 patients with a primary care visit, 31 600 patients (81.3%) underwent screening. Mean (SD) age was 46.2 (15.4) years, and most were aged 35 to 54 years (12 987 [41.1%]), female (18 436 [58.3%]), Hispanic (14 809 [46.9%]), and English-speaking (22 519 [71.3%]), and had Medicaid insurance (18 442 [58.4%]). A total of 10 262 participants (32.5%) screened positive and, of these, 9701 (94.5%) completed the PEG questionnaire. PEG responses indicated severe pain interference with activities of daily living (PEG ≥7) in 5735 (59.1%) participants. A chronic painful condition had not been diagnosed in 4257 (43.9%) patients in the year before screening. A new chronic painful condition was diagnosed at screening or within 90 days in 2250 (52.9%) patients. Care teams found the workflow acceptable, but cited lengthy administration time, challenges with comprehension of the PEG questions, and limited comprehensiveness as implementation barriers.
Conclusions and relevance: A systematic, 2-step process for chronic pain screening and functional assessment in primary care appeared to identify patients with previously undocumented chronic pain and was feasible to implement. Patient-provided information on the frequency of pain, pain level, and pain interference can help improve the assessment and monitoring of pain in primary care.
Conflict of interest statement
Figures
References
-
- World Health Organization . Musculoskeletal conditions. February 8, 2021. Accessed May 13, 2021. https://www.who.int/news-room/fact-sheets/detail/musculoskeletal-conditions
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

