Percutaneous dilatational tracheotomy in high-risk ICU patients
- PMID: 34319491
- PMCID: PMC8319261
- DOI: 10.1186/s13613-021-00906-5
Percutaneous dilatational tracheotomy in high-risk ICU patients
Abstract
Background: Percutaneous dilatational tracheotomy (PDT) has become an established procedure in intensive care units (ICU). However, the safety of this method has been under debate given the growing number of critically ill patients with high bleeding risk receiving anticoagulation, dual antiplatelet therapy (DAPT) or even a combination of both, i.e. triple therapy. Therefore, the purpose of this study, including such a high proportion of patients on antithrombotic therapy, was to investigate whether PDT in high-risk ICU patients is associated with elevated procedural complications and to analyse the risk factors for bleeding occurring during and after PDT.
Methods: PDT interventions conducted in ICUs at 12 European sites between January 2016 and October 2019 were retrospectively analysed for procedural complications. For subgroup analyses, patient stratification into clinically relevant risk groups based on anticoagulation and antiplatelet treatment regimens was performed and the predictors of bleeding occurrence were analysed.
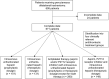
Results: In total, 671 patients receiving PDT were included and stratified into four clinically relevant antithrombotic treatment groups: (1) intravenous unfractionated heparin (iUFH, prophylactic dosage) (n = 101); (2) iUFH (therapeutic dosage) (n = 131); (3) antiplatelet therapy (aspirin and/or P2Y12 receptor inhibitor) with iUFH (prophylactic or therapeutic dosage) except for triple therapy (n = 290) and (4) triple therapy (DAPT with iUFH in therapeutic dosage) (n = 149). Within the whole cohort, 74 (11%) bleedings were reported to be procedure-related. Bleeding occurrence during and after PDT was independently associated with low platelet count (OR 0.73, 95% CI [0.56, 0.92], p = 0.009), chronic kidney disease (OR 1.75, 95% CI [1.01, 3.03], p = 0.047) and previous stroke (OR 2.13, 95% CI [1.1, 3.97], p = 0.02).
Conclusion: In this international, multicenter study bronchoscopy-guided PDT was a safe and low-complication airway management option, even in a cohort of high risk for bleeding on cardiovascular ICUs. Low platelet count, chronic kidney disease and previous stroke were identified as independent risk factors of bleeding during and after PDT but not triple therapy.
Keywords: Airway management; Anticoagulation; Bleeding; Dual antiplatelet therapy; Percutaneous dilatational tracheotomy.
© 2021. The Author(s).
Conflict of interest statement
Martin Orban has received speaker honoraria from Abbott Medical, AstraZeneca, Abiomed, Bayer vital, Biotronik, Bristol-Myers Squibb, CytoSorbents, Daiichi Sankyo Deutschland, Edwards Lifesciences Services, Sedana Medical, outside the submitted work; Rainer Okrojek received speaker honoraria from AstraZeneca, outside the submitted work; Friedhelm Peltz received travel grants and speaker honoraria from Astra Zeneca, Actelion, Novartis, GlaxoSmithKline and Grifols, outside the submitted work. The other authors declare no competing interests.
Figures

Similar articles
-
Safety of Percutaneous Dilatational Tracheotomy in Patients on Dual Antiplatelet Therapy and Anticoagulation.Crit Care Explor. 2019 Oct 30;1(10):e0050. doi: 10.1097/CCE.0000000000000050. eCollection 2019 Oct. Crit Care Explor. 2019. PMID: 32166231 Free PMC article.
-
Endoscopic percutaneous dilatational tracheotomy: a prospective evaluation of 500 consecutive cases.Laryngoscope. 2005 Oct;115(10 Pt 2):1-30. doi: 10.1097/01.MLG.0000163744.89688.E8. Laryngoscope. 2005. PMID: 16227862 Review.
-
Dual antiplatelet therapy after percutaneous left atrial appendage occlusion: single center experience with the Amplatzer Cardiac Plug.Acta Cardiol. 2019 Feb;74(1):74-81. doi: 10.1080/00015385.2018.1455946. Epub 2018 Apr 1. Acta Cardiol. 2019. PMID: 29607737
-
Anticoagulation management around percutaneous bedside procedures: is adjustment required?J Trauma Acute Care Surg. 2012 Apr;72(4):815-20; quiz 1124-5. doi: 10.1097/TA.0b013e31824fbadf. J Trauma Acute Care Surg. 2012. PMID: 22491591
-
Short dual antiplatelet therapy followed by P2Y12 inhibitor monotherapy vs. prolonged dual antiplatelet therapy after percutaneous coronary intervention with second-generation drug-eluting stents: a systematic review and meta-analysis of randomized clinical trials.Eur Heart J. 2021 Jan 21;42(4):308-319. doi: 10.1093/eurheartj/ehaa739. Eur Heart J. 2021. PMID: 33284979
Cited by
-
Authors Response: Safety Analysis of Visual Percutaneous Tracheostomy in Neurocritical Care Patients with Anticoagulation and Antithrombosis.Neurocrit Care. 2025 Aug;43(1):359-360. doi: 10.1007/s12028-025-02256-7. Epub 2025 Apr 11. Neurocrit Care. 2025. PMID: 40214885 No abstract available.
-
Evaluation of the Safety of Percutaneous Dilatational Tracheostomies in Patients with Antiplatelet Therapy-A Comparison of Two Single-Step Percutaneous Dilatational Techniques.J Clin Med. 2025 Jul 16;14(14):5036. doi: 10.3390/jcm14145036. J Clin Med. 2025. PMID: 40725726 Free PMC article.
-
Antiplatelet and anticoagulation use and risk of bleeding from percutaneous dilatational tracheostomy insertion: Systematic review and meta-analysis.J Intensive Care Soc. 2025 Feb 3;26(2):172-182. doi: 10.1177/17511437251314298. eCollection 2025 May. J Intensive Care Soc. 2025. PMID: 39911516 Free PMC article.
-
Common carotid artery distortion before percutaneous dilatational tracheostomy.World J Emerg Med. 2022;13(3):242-244. doi: 10.5847/wjem.j.1920-8642.2022.044. World J Emerg Med. 2022. PMID: 35646221 Free PMC article. No abstract available.
-
Hemorrhages and risk factors in patients undergoing thromboprophylaxis in a respiratory critical care unit: a secondary data analysis of a cohort study.J Intensive Care. 2024 Oct 29;12(1):43. doi: 10.1186/s40560-024-00756-w. J Intensive Care. 2024. PMID: 39473017 Free PMC article.
References
-
- Barbetti JK, Nichol AD, Choate KR, et al. Prospective observational study of postoperative complications after percutaneous dilatational or surgical tracheostomy in critically ill patients. Crit Care Resusc. 2009;11:244–249. - PubMed
LinkOut - more resources
Full Text Sources

