Addressing vaccine hesitancy and access barriers to achieve persistent progress in Israel's COVID-19 vaccination program
- PMID: 34340714
- PMCID: PMC8326649
- DOI: 10.1186/s13584-021-00481-x
Addressing vaccine hesitancy and access barriers to achieve persistent progress in Israel's COVID-19 vaccination program
Abstract
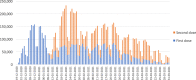
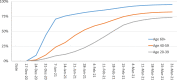
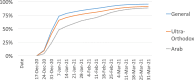
As of March 31, 2021, Israel had administered 116 doses of vaccine for COVID-19 per 100 population (of any age) - far more than any other OECD country. It was also ahead of other OECD countries in terms of the share of the population that had received at least one vaccination (61%) and the share that had been fully vaccinated (55%). Among Israelis aged 16 and over, the comparable figures were 81 and 74%, respectively. In light of this, the objectives of this article are: 1. To describe and analyze the vaccination uptake through the end of March 2021 2. To identify behavioral and other barriers that likely affected desire or ability to be vaccinated 3. To describe the efforts undertaken to overcome those barriers Israel's vaccination campaign was launched on December 20, and within 2.5 weeks, 20% of Israelis had received their first dose. Afterwards, the pace slowed. It took an additional 4 weeks to increase from 20 to 40% and yet another 6 weeks to increase from 40 to 60%. Initially, uptake was low among young adults, and two religious/cultural minority groups - ultra-Orthodox Jews and Israeli Arabs, but their uptake increased markedly over time.In the first quarter of 2021, Israel had to enhance access to the vaccine, address a moderate amount of vaccine hesitancy in its general population, and also address more intense pockets of vaccine hesitancy among young adults and religious/cultural minority groups. A continued high rate of infection during the months of February and March, despite broad vaccination coverage at the time, created confusion about vaccine effectiveness, which in turn contributed to vaccine hesitancy. Among Israeli Arabs, some residents of smaller villages encountered difficulties in reaching vaccination sites, and that also slowed the rate of vaccination.The challenges were addressed via a mix of messaging, incentives, extensions to the initial vaccine delivery system, and other measures. Many of the measures addressed the general population, while others were targeted at subgroups with below-average vaccination rates. Once the early adopters had been vaccinated, it took hard, creative work to increase population coverage from 40 to 60% and beyond.Significantly, some of the capacities and strategies that helped Israel address vaccine hesitancy and geographic access barriers are different from those that enabled it to procure, distribute and administer the vaccines. Some of these strategies are likely to be relevant to other countries as they progress from the challenges of securing an adequate vaccine supply and streamlining distribution to the challenge of encouraging vaccine uptake.
© 2021. The Author(s).
Conflict of interest statement
Three of the authors of this article are IJHPR editors. Accordingly, they were not involved in the editorial aspects of the review process. Instead, the review process was managed by the IJHPR’s associate editor, who is not an author of this article.
Figures
Similar articles
-
Israel's rapid rollout of vaccinations for COVID-19.Isr J Health Policy Res. 2021 Jan 26;10(1):6. doi: 10.1186/s13584-021-00440-6. Isr J Health Policy Res. 2021. PMID: 33499905 Free PMC article.
-
Ethnic and minority group differences in engagement with COVID-19 vaccination programmes - at Pandemic Pace; when vaccine confidence in mass rollout meets local vaccine hesitancy.Isr J Health Policy Res. 2021 May 27;10(1):33. doi: 10.1186/s13584-021-00467-9. Isr J Health Policy Res. 2021. PMID: 34044891 Free PMC article.
-
Developing and validating a culturally tailored questionnaire to assess COVID-19 vaccine hesitancy in Israel's ultraorthodox Jewish population.Hum Vaccin Immunother. 2024 Dec 31;20(1):2429233. doi: 10.1080/21645515.2024.2429233. Epub 2024 Dec 5. Hum Vaccin Immunother. 2024. PMID: 39635713 Free PMC article.
-
Addressing vaccine hesitancy and resistance for COVID-19 vaccines.Int J Nurs Stud. 2022 Jul;131:104241. doi: 10.1016/j.ijnurstu.2022.104241. Epub 2022 Apr 1. Int J Nurs Stud. 2022. PMID: 35489108 Free PMC article. Review.
-
[THE NEED FOR REDUCING DISPARITIES IN SARS-COV-2 IMMUNIZATION: THE ULTRAORTHODOX AND ARAB POPULATIONS IN ISRAEL].Harefuah. 2021 May;160(5):285-290. Harefuah. 2021. PMID: 34028219 Review. Hebrew.
Cited by
-
Impact of implemented vaccination strategies on vaccine uptake and attitude of final year pharmacy students toward COVID-19 vaccines in Gezira State, Sudan.Vaccine X. 2023 Nov 28;15:100416. doi: 10.1016/j.jvacx.2023.100416. eCollection 2023 Dec. Vaccine X. 2023. PMID: 38075433 Free PMC article.
-
Overcoming the effect of pandemic fatigue on vaccine hesitancy-Will belief in science triumph?J Nurs Scholarsh. 2023 Jan;55(1):262-271. doi: 10.1111/jnu.12778. Epub 2022 Apr 7. J Nurs Scholarsh. 2023. PMID: 35388958 Free PMC article.
-
Trends in COVID-19 Vaccination Intent, Determinants and Reasons for Vaccine Hesitancy: Results from Repeated Cross-Sectional Surveys in the Adult General Population of Greece during November 2020-June 2021.Vaccines (Basel). 2022 Mar 18;10(3):470. doi: 10.3390/vaccines10030470. Vaccines (Basel). 2022. PMID: 35335102 Free PMC article.
-
Willingness to be vaccinated against COVID-19 is equal in individuals with affective disorders and healthy controls.Vaccine X. 2022 Aug;11:100186. doi: 10.1016/j.jvacx.2022.100186. Epub 2022 Jun 20. Vaccine X. 2022. PMID: 35755141 Free PMC article.
-
Rational and irrational vaccine hesitancy.Isr J Health Policy Res. 2023 Mar 28;12(1):11. doi: 10.1186/s13584-023-00560-1. Isr J Health Policy Res. 2023. PMID: 36978105 Free PMC article.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials