Mental health among healthcare workers and other vulnerable groups during the COVID-19 pandemic and other coronavirus outbreaks: A rapid systematic review
- PMID: 34347812
- PMCID: PMC8336853
- DOI: 10.1371/journal.pone.0254821
Mental health among healthcare workers and other vulnerable groups during the COVID-19 pandemic and other coronavirus outbreaks: A rapid systematic review
Abstract
Introduction: Although most countries and healthcare systems worldwide have been affected by the COVID-19 pandemic, some groups of the population may be more vulnerable to detrimental effects of the pandemic on mental health than others. The aim of this systematic review was to synthesise evidence currently available from systematic reviews on the impact of COVID-19 and other coronavirus outbreaks on mental health for groups of the population thought to be at increased risk of detrimental mental health impacts.
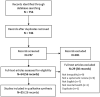
Materials and methods: We conducted a systematic review of reviews on adults and children residing in a country affected by a coronavirus outbreak and belonging to a group considered to be at risk of experiencing mental health inequalities. Data were collected on symptoms or diagnoses of any mental health condition, quality of life, suicide or attempted suicide. The protocol for this systematic review was registered in the online PROSPERO database prior to commencing the review (https://www.crd.york.ac.uk/prospero/display_record.php?RecordID=194264).
Results: We included 25 systematic reviews. Most reviews included primary studies of hospital workers from multiple countries. Reviews reported variable estimates for the burden of symptoms of mental health problems among acute healthcare workers, COVID-19 patients with physical comorbidities, and children and adolescents. No evaluations of interventions were identified. Risk- and protective factors, mostly for healthcare workers, showed the importance of personal factors, the work environment, and social networks for mental health.
Conclusions: This review of reviews based on primary studies conducted in the early months of the COVID-19 pandemic shows a lack of evidence on mental health interventions and mental health impacts on vulnerable groups in the population.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Mental burden and its risk and protective factors during the early phase of the SARS-CoV-2 pandemic: systematic review and meta-analyses.Global Health. 2021 Mar 29;17(1):34. doi: 10.1186/s12992-021-00670-y. Global Health. 2021. PMID: 33781283 Free PMC article.
-
Factors affecting mental health of health care workers during coronavirus disease outbreaks (SARS, MERS & COVID-19): A rapid systematic review.PLoS One. 2020 Dec 15;15(12):e0244052. doi: 10.1371/journal.pone.0244052. eCollection 2020. PLoS One. 2020. PMID: 33320910 Free PMC article.
-
Impact of COVID-19 pandemic on mental health of young people and adults: a systematic review protocol of observational studies.BMJ Open. 2020 Jul 1;10(7):e039426. doi: 10.1136/bmjopen-2020-039426. BMJ Open. 2020. PMID: 32611746 Free PMC article.
-
Impact and Mechanism of Covid-19 on Mental Health and Wellbeing.Ir Med J. 2020 Jun 11;113(6):100. Ir Med J. 2020. PMID: 32816435
-
Psychological impact of an epidemic/pandemic on the mental health of healthcare professionals: a rapid review.BMC Public Health. 2020 Aug 12;20(1):1230. doi: 10.1186/s12889-020-09322-z. BMC Public Health. 2020. PMID: 32787815 Free PMC article.
Cited by
-
The Elephant in the Room: A Cross-Sectional Study on the Stressful Psychological Effects of the COVID-19 Pandemic in Mental Healthcare Workers.Brain Sci. 2022 Mar 19;12(3):408. doi: 10.3390/brainsci12030408. Brain Sci. 2022. PMID: 35326364 Free PMC article.
-
Changes in Mental Health Needs during COVID-19 in the Republic of Georgia: A Longitudinal Follow-up Study.Clin Pract Epidemiol Ment Health. 2022 Aug 22;18:e174501792208100. doi: 10.2174/17450179-v18-e2208100. eCollection 2022. Clin Pract Epidemiol Ment Health. 2022. PMID: 37274862 Free PMC article.
-
Nursing Staff in a Large Hospital System Underutilize Insurance-Based Mental Health Services.Healthcare (Basel). 2024 Jun 13;12(12):1188. doi: 10.3390/healthcare12121188. Healthcare (Basel). 2024. PMID: 38921306 Free PMC article.
-
Mental health and health-related quality of life among healthcare workers in Indonesia during the COVID-19 pandemic: a cross-sectional study.BMJ Open. 2022 Apr 8;12(4):e057963. doi: 10.1136/bmjopen-2021-057963. BMJ Open. 2022. PMID: 35396304 Free PMC article.
-
Evaluation of Health-Related Quality of Life and Mental Health in 729 Medical Students in Indonesia During the COVID-19 Pandemic.Med Sci Monit. 2023 Feb 9;29:e938892. doi: 10.12659/MSM.938892. Med Sci Monit. 2023. PMID: 36755476 Free PMC article.
References
-
- Mental Health Foundation. Coronavirus. The divergence of mental health experiences during the pandemic. Mental Health in the Pandemic Series. 2020. https://www.mentalhealth.org.uk/sites/default/files/MHF%20The%20COVID-19....
-
- Nobles J, Martin F, Dawson S, Moran P, Savovic J. The potential impact of COVID-19 on mental health outcomes and the implications for service solutions. 15 April 2020. https://arc-w.nihr.ac.uk/covid-response/rapid-reports/potential-impact-o....
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical