A standardized definition of placental infection by SARS-CoV-2, a consensus statement from the National Institutes of Health/Eunice Kennedy Shriver National Institute of Child Health and Human Development SARS-CoV-2 Placental Infection Workshop
- PMID: 34364845
- PMCID: PMC8340595
- DOI: 10.1016/j.ajog.2021.07.029
A standardized definition of placental infection by SARS-CoV-2, a consensus statement from the National Institutes of Health/Eunice Kennedy Shriver National Institute of Child Health and Human Development SARS-CoV-2 Placental Infection Workshop
Erratum in
-
December 2021 (vol. 225, no. 6, page 593).Am J Obstet Gynecol. 2023 Jan;228(1):124. doi: 10.1016/j.ajog.2022.03.005. Epub 2022 Apr 18. Am J Obstet Gynecol. 2023. PMID: 35440371 Free PMC article. No abstract available.
Abstract
Pregnant individuals infected with SARS-CoV-2 have higher rates of intensive care unit admission, oxygen requirement, need for mechanical ventilation, and death than nonpregnant individuals. Increased COVID-19 disease severity may be associated with an increased risk of viremia and placental infection. Maternal SARS-CoV-2 infection is also associated with pregnancy complications such as preeclampsia and preterm birth, which can be either placentally mediated or reflected in the placenta. Maternal viremia followed by placental infection may lead to maternal-fetal transmission (vertical), which affects 1% to 3% of exposed newborns. However, there is no agreed-upon or standard definition of placental infection. The National Institutes of Health/Eunice Kennedy Shriver National Institute of Child Health and Human Development convened a group of experts to propose a working definition of placental infection to inform ongoing studies of SARS-CoV-2 during pregnancy. Experts recommended that placental infection be defined using techniques that allow virus detection and localization in placental tissue by one or more of the following methods: in situ hybridization with antisense probe (detects replication) or a sense probe (detects viral messenger RNA) or immunohistochemistry to detect viral nucleocapsid or spike proteins. If the abovementioned methods are not possible, reverse transcription polymerase chain reaction detection or quantification of viral RNA in placental homogenates, or electron microscopy are alternative approaches. A graded classification for the likelihood of placental infection as definitive, probable, possible, and unlikely was proposed. Manuscripts reporting placental infection should describe the sampling method (location and number of samples collected), method of preservation of tissue, and detection technique. Recommendations were made for the handling of the placenta, examination, and sampling and the use of validated reagents and sample protocols (included as appendices).
Keywords: COVID-19; SARS-CoV-2; fetal death; immunohistochemistry; in situ hybridization; placental infection; placentitis; preeclampsia; preterm birth; stillbirth; syncytiotrophoblast; vertical transmission.
Copyright © 2021 Elsevier Inc. All rights reserved.
Figures

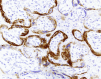

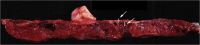

References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

