Case Report: Iatrogenic Dental Progress of Phantom Bite Syndrome: Rare Cases With the Comorbidity of Psychosis
- PMID: 34366932
- PMCID: PMC8334004
- DOI: 10.3389/fpsyt.2021.701232
Case Report: Iatrogenic Dental Progress of Phantom Bite Syndrome: Rare Cases With the Comorbidity of Psychosis
Abstract
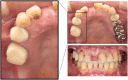
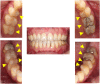
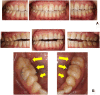
Introduction: Phantom bite syndrome (PBS) is considered as the preoccupation with dental occlusion and the continual inability to adapt to changed occlusion. These patients constantly demand occlusal corrections and undergo extensive and excessive dental treatments. We present three cases with PBS-suspected iatrogenic concerns and the attribution to underlying psychosis. Case Presentation: A 70-year-old female demanded orthodontic retreatment and complained of tightness and cramped sensation of teeth in the oral cavity, uncomfortable occlusion, and pain in her neck and legs that she was convinced was induced by orthodontic treatment. However, even earlier than the orthodontic treatment, she had kept doctor shopping for over 35 years, not merely dentists but also psychiatrists, neurologists, and so on; she was diagnosed with bipolar disorder. A 48-year-old female complained of malaligned improper occlusion and demanded occlusal adjustment. These symptoms occurred in the absence of a dental trigger and were worsened by orthodontic treatment. She underwent psychiatric treatment for 15 years with a diagnosis of bipolar disorder. A 38-year-old female, who had a history of schizophrenia for over 20 years, complained of occlusal discomfort and revisited with a complaint of abnormal occlusion due to excessive dental procedures. In the last two cases, requests for dental procedures had reduced owing to the collaboration between the psychiatrists and dentists. All the cases first visited our clinic following a succession of dental visits. They were strongly convinced that occlusal correction was the only solution to their symptoms, including the symptoms of discomfort in other body parts. Their misleading perceptions were uncorrectable, and repeated dental treatments exacerbated their complaints. Moreover, the dentists overlooked the psychotic histories of the patients, while the comorbid psychosis resulted in a strict demand for dental treatment by the patients. Conclusions: The presented PBS cases with psychosis suggest that repeated dental treatments and comorbid psychosis exacerbate PBS. Moreover, their persistent demands reflecting comorbid psychosis led dentists to perform numerous procedures. Early detection of underlying psychosis and the prompt collaboration between psychiatrists and dentists are integral to help prevent complications in PBS cases with psychosis.
Keywords: bipolar disorder; case report; medical collaboration; occlusal dysesthesia; phantom bite syndrome; psychiatric background; psychosis; schizophrenia.
Copyright © 2021 Watanabe, Hong, Liu, Takao, Suga, Tu, Yoshikawa, Takenoshita, Sato, Higashihori, Moriyama, Motomura and Toyofuku.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Comorbid depressive disorders and left-side dominant occlusal discomfort in patients with phantom bite syndrome.J Oral Rehabil. 2020 Jan;47(1):36-41. doi: 10.1111/joor.12872. Epub 2019 Aug 28. J Oral Rehabil. 2020. PMID: 31398263 Free PMC article.
-
Phantom bite: a case report and literature review.Cranio. 2015 Jul;33(3):228-31. doi: 10.1179/2151090314Y.0000000002. Epub 2014 Apr 30. Cranio. 2015. PMID: 26159690 Review.
-
Psychiatric comorbidities and psychopharmacological outcomes of phantom bite syndrome.J Psychosom Res. 2015 Mar;78(3):255-9. doi: 10.1016/j.jpsychores.2014.11.010. Epub 2014 Nov 15. J Psychosom Res. 2015. PMID: 25477300
-
[Advance in research of occlusal dysesthesia].Zhonghua Kou Qiang Yi Xue Za Zhi. 2021 Jan 9;56(1):109-112. doi: 10.3760/cma.j.cn112144-20200328-00175. Zhonghua Kou Qiang Yi Xue Za Zhi. 2021. PMID: 34645246 Chinese.
-
Phantom bite syndrome: Revelation from clinically focused review.World J Psychiatry. 2021 Nov 19;11(11):1053-1064. doi: 10.5498/wjp.v11.i11.1053. eCollection 2021 Nov 19. World J Psychiatry. 2021. PMID: 34888173 Free PMC article. Review.
Cited by
-
Case series of drug-induced open bite: Extrapyramidal symptoms related to psychotropic medications.Front Psychiatry. 2023 Mar 28;14:1137917. doi: 10.3389/fpsyt.2023.1137917. eCollection 2023. Front Psychiatry. 2023. PMID: 37056404 Free PMC article.
-
Case report: Long-term management of occlusion after surgical-orthodontic treatment for a patient with drug-induced open bite developed after the onset of schizophrenia.Front Psychiatry. 2023 Dec 19;14:1304215. doi: 10.3389/fpsyt.2023.1304215. eCollection 2023. Front Psychiatry. 2023. PMID: 38173706 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources

