Insulin Treatment May Increase Adverse Outcomes in Patients With COVID-19 and Diabetes: A Systematic Review and Meta-Analysis
- PMID: 34367067
- PMCID: PMC8339900
- DOI: 10.3389/fendo.2021.696087
Insulin Treatment May Increase Adverse Outcomes in Patients With COVID-19 and Diabetes: A Systematic Review and Meta-Analysis
Abstract
Background and objective: Recently, insulin treatment has been found to be associated with increased mortality and other adverse outcomes in patients with coronavirus disease 2019 (COVID-19) and diabetes, but the results remain unclear and controversial, therefore, we conducted this meta-analysis.
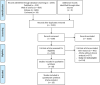
Methods: Four databases, namely, PubMed, Web of Science, EMBASE and the Cochrane Library, were used to identify all studies concerning insulin treatment and the adverse effects of COVID-19, including mortality, incidence of severe/critical complications, in-hospital admission and hospitalization time. To assess publication bias, funnel plots, Begg's tests and Egger's tests were used. The odds ratios (ORs) with 95% confidence intervals (CIs) were used to access the effect of insulin therapy on mortality, severe/critical complications and in-hospital admission. The association between insulin treatment and hospitalization time was calculated by the standardized mean difference (SMD) with 95% CIs.
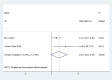
Results: Eighteen articles, involving a total of 12277 patients with COVID-19 and diabetes were included. Insulin treatment was significantly associated with an increased risk of mortality (OR=2.10; 95% CI, 1.51-2.93) and incidence of severe/critical COVID-19 complications (OR=2.56; 95% CI, 1.18-5.55). Moreover, insulin therapy may increase in-hospital admission in patients with COVID-19 and diabetes (OR=1.31; 95% CI, 1.06-1.61). However, there was no significant difference in the hospitalization time according to insulin treatment (SMD=0.21 95% CI, -0.02-0.45).
Conclusions: Insulin treatment may increase mortality and severe/critical complications in patients with COVID-19 and diabetes, but more large-scale studies are needed to confirm and explore the exact mechanism.
Keywords: COVID-19; adverse outcomes; complications; diabetes; insulin treatment; mortality.
Copyright © 2021 Yang, Cai and Zhang.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures





Similar articles
-
DPP-4 inhibitors may improve the mortality of coronavirus disease 2019: A meta-analysis.PLoS One. 2021 May 20;16(5):e0251916. doi: 10.1371/journal.pone.0251916. eCollection 2021. PLoS One. 2021. PMID: 34015003 Free PMC article.
-
(Ultra-)long-acting insulin analogues for people with type 1 diabetes mellitus.Cochrane Database Syst Rev. 2021 Mar 4;3(3):CD013498. doi: 10.1002/14651858.CD013498.pub2. Cochrane Database Syst Rev. 2021. PMID: 33662147 Free PMC article.
-
Mortality and other adverse outcomes in patients with type 2 diabetes mellitus admitted for COVID-19 in association with glucose-lowering drugs: a nationwide cohort study.BMC Med. 2020 Nov 16;18(1):359. doi: 10.1186/s12916-020-01832-2. BMC Med. 2020. PMID: 33190637 Free PMC article.
-
Clinical characteristics and risk factors of infection in patients with systemic lupus erythematosus: A systematic review and meta-analysis of observational studies.Semin Arthritis Rheum. 2020 Oct;50(5):1022-1039. doi: 10.1016/j.semarthrit.2020.06.004. Epub 2020 Jun 17. Semin Arthritis Rheum. 2020. PMID: 32911280
-
Hyperglycemia at admission is a strong predictor of mortality and severe/critical complications in COVID-19 patients: a meta-analysis.Biosci Rep. 2021 Feb 26;41(2):BSR20203584. doi: 10.1042/BSR20203584. Biosci Rep. 2021. PMID: 33480978 Free PMC article.
Cited by
-
COVID-19 and Diabetes Outcomes: Rationale for and Updates from the CORONADO Study.Curr Diab Rep. 2022 Feb;22(2):53-63. doi: 10.1007/s11892-022-01452-5. Curr Diab Rep. 2022. PMID: 35171448 Free PMC article. Review.
-
"Hyperglycemic Memory": Observational Evidence to Experimental Inference.Curr Diabetes Rev. 2025;21(4):64-78. doi: 10.2174/0115733998279869231227091944. Curr Diabetes Rev. 2025. PMID: 38369731 Review.
-
Diabetes Mellitus and Multidrug-Resistant Gram-Negative Bacterial Infections in Critically Ill COVID-19 Patients: A Retrospective Observational Study.Diagnostics (Basel). 2025 May 8;15(10):1190. doi: 10.3390/diagnostics15101190. Diagnostics (Basel). 2025. PMID: 40428183 Free PMC article.
-
Insulin use in type II diabetic patients: a predictive of mortality in covid-19 infection.Diabetol Metab Syndr. 2022 Jun 20;14(1):85. doi: 10.1186/s13098-022-00857-2. Diabetol Metab Syndr. 2022. PMID: 35725489 Free PMC article.
-
COVID-19 and Gestational Diabetes: The Role of Nutrition and Pharmacological Intervention in Preventing Adverse Outcomes.Nutrients. 2022 Aug 30;14(17):3562. doi: 10.3390/nu14173562. Nutrients. 2022. PMID: 36079820 Free PMC article. Review.
References
-
- Bhadade R, Harde M, deSouza R, Kasbe A, Deshpande C, Dave S, et al. . Appraisal of Critically Ill COVID-19 Patients at a Dedicated COVID Hospital The Effects of Type 2 Diabetes Mellitus on Organ Metabolism and the Immune System. J Assoc Phys India (2020) 68(9):14–9. 10.1016/s2213-8587(20)30271-0 - DOI - PubMed
-
- Wang S, Ma P, Zhang S, Song S, Wang Z, Ma Y, et al. . Fasting Blood Glucose at Admission is an Independent Predictor for 28-Day Mortality in Patients With COVID-19 Without Previous Diagnosis of Diabetes: A Multi-Centre Retrospective Study. Diabetologia (2020) 63(10):2102–11. 10.1007/s00125-020-05209-1 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

