Virtual Simulation for Interactive Visualization of 3D Fracture Fixation Biomechanics
- PMID: 34370717
- PMCID: PMC8692361
- DOI: 10.5435/JAAOS-D-20-01322
Virtual Simulation for Interactive Visualization of 3D Fracture Fixation Biomechanics
Abstract
Introduction: In the surgical fixation of fractures, proper biomechanical stability is key in preventing clinical complications including poor fracture healing, residual deformity, loss of fixation, or implant failure. Stability is largely influenced by treatment decisions made by the surgeon. The interplay of surgeon-controlled variables and their effect on the three-dimensional (3D) biomechanics of a fracture fixation construct are often not intuitive, and current training methods do not facilitate a deep understanding of these interactions.
Methods: A simulation software interface, FracSim, was developed. FracSim is built on a large precomputed library of finite element simulations. The software allows a surgeon to make adjustments to a virtual fracture fixation construct/weight-bearing plan and immediately visualize how these changes affect 3D biomechanics, including implant stress and fracture gap strain, important for clinical success. Twenty-one orthopaedic residents completed an instructor-led educational session with FracSim focused on bridge plating. Subjects completed pretests and posttests of knowledge of biomechanical concepts and a questionnaire.
Results: Subjects scored a mean of 5.6/10 on the pretest of biomechanical knowledge. Senior residents scored better than junior residents (P = 0.04). After the educational session with FracSim, residents improved their test scores to a mean of 8.0/10, with a significant improvement (P < 0.001). Questionnaire scores indicated that subjects believed that FracSim had realistic implants, constructs, and motions and that training with FracSim was purposeful, desirable, efficient, fun, and useful for enhancing the understanding of fracture fixation biomechanics.
Discussion: This new type of simulation software enables interactive visualization of 3D fracture fixation biomechanics. Limitations of this study include lack of a control group undergoing traditional education and lack of a delayed posttest to assess retention. FracSim may provide an effective and engaging way to promote a deeper understanding of biomechanical concepts in the orthopaedic learner.
Copyright © 2021 by the American Academy of Orthopaedic Surgeons.
Figures


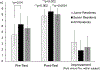
References
-
- Atesok K, Mabrey JD, Jazrawi LM & Egol KA Surgical simulation in orthopaedic skills training. J. Am. Acad. Orthop. Surg 20, 410–422 (2012). - PubMed
-
- Ruikar DD, Hegadi RS & Santosh KC A Systematic Review on Orthopedic Simulators for Psycho-Motor Skill and Surgical Procedure Training. J. Med. Syst 42, 168 (2018). - PubMed
-
- Bartlett JD, Lawrence JE, Stewart ME, Nakano N & Khanduja V Does virtual reality simulation have a role in training trauma and orthopaedic surgeons? Bone Jt. J 100-B, 559–565 (2018). - PubMed
-
- Negrillo-Cárdenas J, Jiménez-Pérez J-R & Feito FR The role of virtual and augmented reality in orthopedic trauma surgery: From diagnosis to rehabilitation. Comput. Methods Programs Biomed 191, 105407 (2020). - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

