Adaptive Treatment for Youth With Substance Use and Depression: Early Depression Response and Short-term Outcomes
- PMID: 34371102
- PMCID: PMC8818057
- DOI: 10.1016/j.jaac.2021.07.807
Adaptive Treatment for Youth With Substance Use and Depression: Early Depression Response and Short-term Outcomes
Abstract
Objective: To investigate prevalence and predictors of early depression response (EDR) in adolescents with substance use and depression receiving cognitive-behavioral therapy (CBT) for substance use and to test the efficacy of supplemental CBT targeting depression (CBT-D) for non-EDR adolescents in an adaptive treatment approach.
Method: At 2 sites, 95 youths (ages 14-21, mean [SD] = 17.4 [1.8]) with alcohol or cannabis use and depressive symptoms received up to 12 sessions of CBT for substance use over 14 weeks. Assessments were at baseline and weeks 4, 9, and 14. The Children's Depression Rating Scale-Revised was the primary depression measure, with a reduction of 50% or more on this scale at week 4 defining EDR. The primary substance use outcomes of alcohol use, heavy alcohol use, and cannabis use frequency were assessed via interview report on the Alcohol Consumption Questionnaire and the Drug Checklist. Urinalysis provided a secondary measure of cannabis use. Non-EDR adolescents were randomly assigned to supplemental CBT-D or enhanced treatment as usual (ETAU).
Results: Thirty-five adolescents (37%; 95% CI, 27%-47%) demonstrated EDR. Fewer days of cannabis use (odds ratio 0.977; 95% CI, 0.961-0.992) and absence of conduct disorder (odds ratio 0.149; 95% CI, 0.031-0.716) predicted EDR. Frequency of drinking (F1,82 = 11.09, η2 = 0.119, p = .001), heavy drinking (F1,82 = 19.91, η2 = 0.195, p < .0001), and cannabis use (F1,220 = 35.01, η2 = 0.137, p < .001) decreased over time for EDR, CBT-D, and ETAU adolescents, with EDR adolescents evidencing earlier lower cannabis use (F2,220 = 4.16, η2 = 0.036, p = .0169). Negative (clean) urine screens increased over time (F1,219 = 5.10, η2 = 0.023, p = .0249). Comparison of CBT-D and ETAU indicated that depression significantly decreased over time in both groups (F1,48 = 64.20, η2 = 0.572, p < .001), with no advantage for CBT-D.
Conclusion: Approximately one-third of adolescents with substance use and depression attain EDR during substance use treatment. Less frequent cannabis use facilitates depression response. The relatively small sample may have precluded identification of additional EDR predictors.
Clinical trial registration information: Treatment for Teens With Alcohol Abuse and Depression; https://clinicaltrials.gov/; NCT02227589.
Keywords: adaptive treatment; adolescence; cognitive-behavioral therapy; depression; substance use.
Copyright © 2021 American Academy of Child and Adolescent Psychiatry. Published by Elsevier Inc. All rights reserved.
Figures
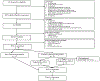


References
-
- Substance Abuse and Mental Health Services Administration. Key Substance Use and Mental Health Indicators in the United States: Results from the 2018 National Survey on Drug Use and Health. Vol 170. (Substance Abuse and Mental Health Services, ed.). Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration.; 2019. https://www.samhsa.gov/data/
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

