Association Between Receipt of Overlapping Opioid and Benzodiazepine Prescriptions From Multiple Prescribers and Overdose Risk
- PMID: 34374769
- PMCID: PMC8356065
- DOI: 10.1001/jamanetworkopen.2021.20353
Association Between Receipt of Overlapping Opioid and Benzodiazepine Prescriptions From Multiple Prescribers and Overdose Risk
Abstract
Importance: The receipt of overlapping opioid and benzodiazepine prescriptions is associated with increased overdose risk. It is unknown whether this increase in risk varies when overlapping prescriptions are written by multiple prescribers vs 1 prescriber.
Objective: To evaluate the association between receipt of overlapping opioid and benzodiazepine prescriptions from multiple prescribers and overdose risk.
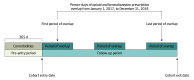
Design, setting, and participants: This cohort study was conducted using 2017 to 2018 claims from the Optum deidentified Clinformatics Data Mart. Participants were patients with private insurance or Medicare Advantage aged 12 years or older with overlapping opioid and benzodiazepine prescriptions. Data were analyzed from March through November 2020.
Exposures: For each patient, person-days on which opioid and benzodiazepine prescriptions overlapped were identified. The exposure was whether these prescriptions were written by multiple prescribers vs 1 prescriber.
Main outcomes and measures: The outcome was a treated overdose, defined as the occurrence of 1 or more claims containing a diagnosis code for opioid or benzodiazepine poisoning on a person-day of opioid-benzodiazepine overlap. The association between exposure and outcome at the person-day level was estimated using logistic regression, controlling for opioid and benzodiazepine prescribing patterns, demographics, and comorbidities. The average marginal effect (AME) of the exposure, defined as the absolute difference in the probability of a treated overdose if all person-days of overlap involved prescriptions from multiple prescribers vs 1 prescriber, was calculated.
Results: Among 529 053 patients, the mean (SD) age was 61.2 (15.6) years and 350 857 (66.3%) were female patients. Mean (SD) follow-up was 198.7 (249.8) days. During follow-up, overdose occurred on 1 or more person-days of opioid-benzodiazepine overlap for 2288 patients (0.4%, or 1 in 231 patients). There were 52 989 316 person-days of opioid-benzodiazepine overlap. Among 19 895 457 person-days (37.5%) involving prescriptions from multiple prescribers, there were 1390 overdoses (7.0 per 100 000 person-days), and among 33 093 859 person-days (62.5%) involving prescriptions from 1 prescriber, there were 1302 overdoses (3.9 per 100 000 person-days). Overdose risk was increased 1.8-fold (95% CI, 1.6-1.9) on person-days of overlap involving prescriptions from multiple prescribers vs 1 prescriber. The association between multiple prescribers and increased risk of overdose persisted in adjusted analyses (adjusted odds ratio, 1.20; 95% CI, 1.10-1.31; AME, 0.91 per 100 000 person-days of overlap; 95% CI, 0.46-1.37).
Conclusions and relevance: This study found that among patients already at increased risk of overdose owing to concurrent treatment with opioids and benzodiazepines, overdose risk was increased further when multiple prescribers were responsible for this treatment regimen compared with 1 prescriber. This increased risk was not fully accounted for by differences in prescribing patterns, demographics, or comorbidities. This finding suggests that other factors, such as poor care coordination, may be associated with the increase in risk.
Conflict of interest statement
Figures

References
-
- Gladden RM, O’Donnell J, Mattson CL, Seth P. Changes in opioid-involved overdose deaths by opioid type and presence of benzodiazepines, cocaine, and methamphetamine—25 States, July-December 2017 to January-June 2018. MMWR Morb Mortal Wkly Rep. 2019;68(34):737-744. doi:10.15585/mmwr.mm6834a2 - DOI - PMC - PubMed

