Pelvic osteotomies for acetabular dysplasia: Are there outcomes, survivorship and complication differences between different osteotomy techniques?
- PMID: 34377519
- PMCID: PMC8349594
- DOI: 10.1093/jhps/hnab009
Pelvic osteotomies for acetabular dysplasia: Are there outcomes, survivorship and complication differences between different osteotomy techniques?
Abstract
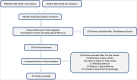
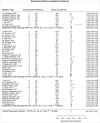
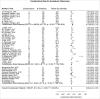
The purpose of this study was to evaluate the safety and efficacy of Periacetabular osteotomy (PAO), rotational acetabular osteotomy (RAO), and eccentric rotational acetabular osteotomy (ERAO) for treating hip dysplasia by comparing complication rates, survivorship, and functional outcomes after treatment. A systematic review in the MEDLINE and CINAHL databases was performed, and studies reporting outcomes after pelvic osteotomy for hip dysplasia with a minimum of 1-year follow-up or reported postoperative complications was included. Patient demographics, radiographic measurements, patient reported outcomes including the modified Harris hip score (mHHS), complications using the modified Clavien-Dindo classification, and reoperations were extracted from each study. A meta-analysis of outcome scores, complications, change in acetabular coverage, and revision rates for the 3 pelvic osteotomies was performed. A total of 47 articles detailing outcomes of 6,107 patients undergoing pelvic osteotomies were included in the final analysis. When stratified by procedure, RAO had a statistically greater change in LCEA when compared to PAO (33.9° vs 18.0°; P <0.001). The average pooled mHHS improvement was 15.6 (95% CI: 8.3-22.8, I 2= 99.4%). Although ERAO had higher mean score improvements when compared to RAO and PAO, the difference was not statistically significant (P >0.05). Lastly, patients undergoing PAO had a statistically greater complication rate than those undergoing ERAO and RAO (P <0.001 for both), while revision rate was not statistically different between the 3 techniques. In summary, there are many more publications on PAO surgery with a wide range of reported complications. Complications after ERAO and RAO surgery are lower than PAO surgery in the literature, but it is unclear whether this represents an actual difference or a reporting bias. Lastly, there are no significant differences between revisions, or postoperative reported outcomes between the 3 techniques.
© The Author(s) 2021. Published by Oxford University Press.
Figures



References
-
- Maquet P. Biomechanics of hip dysplasia. Acta Orthop 1999; 65: 302–14. - PubMed
-
- Hattori T, Inaba Y, Ichinohe S et al. The epidemiology of developmental dysplasia of the hip in Japan: findings from a nationwide multi-center survey. J Orthop Sci 2017; 22: 121–6. - PubMed
-
- Jingushi S, Ohfuji S, Sofue M et al. Osteoarthritis hip joints in Japan: involvement of acetabular dysplasia. J Orthop Sci 2011; 16: 156–64. - PubMed
-
- Ganz R, Klaue K, Vinh TS, Mast JW. A new periacetabular osteotomy for the treatment of hip dysplasias. Technique and preliminary results. Clin Orthop Relat Res 1988; 232: 26–36. - PubMed
LinkOut - more resources
Full Text Sources

