Shape-Sensing Robotic-Assisted Bronchoscopy in the Diagnosis of Pulmonary Parenchymal Lesions
- PMID: 34384789
- PMCID: PMC8941601
- DOI: 10.1016/j.chest.2021.07.2169
Shape-Sensing Robotic-Assisted Bronchoscopy in the Diagnosis of Pulmonary Parenchymal Lesions
Abstract
Background: The landscape of guided bronchoscopy for the sampling of pulmonary parenchymal lesions is evolving rapidly. Shape-sensing robotic-assisted bronchoscopy (ssRAB) recently was introduced as means to allow successful sampling of traditionally challenging lesions.
Research question: What are the feasibility, diagnostic yield, determinants of diagnostic sampling, and safety of ssRAB in patients with pulmonary lesions?
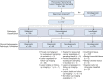
Study design and methods: Data from 131 consecutive ssRAB procedures performed at a US-based cancer center between October 2019 and July 2020 were captured prospectively and analyzed retrospectively. Definitions of diagnostic procedures were based on prior standards. Associations of procedure- and lesion-related factors with diagnostic yield were examined by univariate and multivariate generalized linear mixed models.
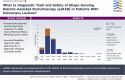
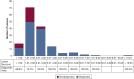
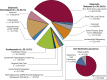
Results: A total of 159 pulmonary lesions were targeted during 131 ssRAB procedures. The median lesion size was 1.8 cm, 59.1% of lesions were in the upper lobe, and 66.7% of lesions were beyond a sixth-generation airway. The navigational success rate was 98.7%. The overall diagnostic yield was 81.7%. Lesion size of ≥ 1.8 cm and central location were associated significantly with a diagnostic procedure in the univariate analysis. In the multivariate model, lesions of ≥ 1.8 cm were more likely to be diagnostic compared with lesions < 1.8 cm, after adjusting for lung centrality (OR, 12.22; 95% CI, 1.66-90.10). The sensitivity and negative predictive value of ssRAB for primary thoracic malignancies were 79.8% and 72.4%, respectively. The overall complication rate was 3.0%, and the pneumothorax rate was 1.5%.
Interpretation: This study was the first to provide comprehensive evidence regarding the usefulness and diagnostic yield of ssRAB in the sampling of pulmonary parenchymal lesions. ssRAB may represent a significant advancement in the ability to access and sample successfully traditionally challenging pulmonary lesions via the bronchoscopic approach, while maintaining a superb safety profile. Lesion size seems to remain the major predictor of a diagnostic procedure.
Keywords: diagnostic yield; pulmonary nodule; robotic-assisted bronchoscopy.
Copyright © 2021 American College of Chest Physicians. Published by Elsevier Inc. All rights reserved.
Figures
Comment in
-
Image-guided Bronchoscopy: Established and Emerging Approaches.Am J Respir Crit Care Med. 2023 Jul 1;208(1):98-100. doi: 10.1164/rccm.202205-1008RR. Am J Respir Crit Care Med. 2023. PMID: 37129567 No abstract available.
Similar articles
-
Shape sensing robotic assisted bronchoscopy versus virtual bronchoscopic navigation in the diagnosis of peripheral pulmonary nodules.Sci Rep. 2025 Jul 4;15(1):23950. doi: 10.1038/s41598-025-08798-2. Sci Rep. 2025. PMID: 40615493 Free PMC article.
-
Shape-Sensing Robotic-Assisted Bronchoscopy vs Digital Tomosynthesis-Corrected Electromagnetic Navigation Bronchoscopy: A Comparative Cohort Study of Diagnostic Performance.Chest. 2023 Apr;163(4):977-984. doi: 10.1016/j.chest.2022.10.019. Epub 2022 Oct 29. Chest. 2023. PMID: 36441041
-
Diagnostic performance of Shape-Sensing Robotic-Assisted bronchoscopy with mobile Cone-Beam CT for cystic and cavitary pulmonary lesions.Lung Cancer. 2024 Dec;198:108029. doi: 10.1016/j.lungcan.2024.108029. Epub 2024 Nov 17. Lung Cancer. 2024. PMID: 39577353
-
Diagnostic Performance and Safety Profile of Robotic-assisted Bronchoscopy: A Systematic Review and Meta-Analysis.Ann Am Thorac Soc. 2023 Dec;20(12):1801-1812. doi: 10.1513/AnnalsATS.202301-075OC. Ann Am Thorac Soc. 2023. PMID: 37769170
-
Tissue diagnosis of suspected lung cancer: selecting between bronchoscopy, transthoracic needle aspiration, and resectional biopsy.Respir Care Clin N Am. 2003 Mar;9(1):51-76. doi: 10.1016/s1078-5337(02)00083-7. Respir Care Clin N Am. 2003. PMID: 12820712 Review.
Cited by
-
Mediastinal Staging in Non-Small-Cell Lung Cancer: Saying Goodbye to Mediastinoscopy.J Clin Oncol. 2023 Aug 1;41(22):3785-3790. doi: 10.1200/JCO.23.00867. Epub 2023 Jun 2. J Clin Oncol. 2023. PMID: 37267507 Free PMC article. Review.
-
Development and deployment of robots in a bronchoscopy suite.Breathe (Sheff). 2025 Jul 15;21(3):240247. doi: 10.1183/20734735.0247-2024. eCollection 2025 Jul. Breathe (Sheff). 2025. PMID: 40673070 Free PMC article. Review.
-
Combining Shape-Sensing Robotic Bronchoscopy With Mobile Three-Dimensional Imaging to Verify Tool-in-Lesion and Overcome Divergence: A Pilot Study.Mayo Clin Proc Innov Qual Outcomes. 2022 Apr 23;6(3):177-185. doi: 10.1016/j.mayocpiqo.2022.02.004. eCollection 2022 Jun. Mayo Clin Proc Innov Qual Outcomes. 2022. PMID: 35509435 Free PMC article.
-
Transbronchial Techniques for Lung Cancer Treatment: Where Are We Now?Cancers (Basel). 2023 Feb 8;15(4):1068. doi: 10.3390/cancers15041068. Cancers (Basel). 2023. PMID: 36831411 Free PMC article. Review.
-
Robotic Assisted Bronchoscopy: The Ultimate Solution for Peripheral Pulmonary Nodules?Respiration. 2022;101(5):437-440. doi: 10.1159/000522516. Epub 2022 Mar 23. Respiration. 2022. PMID: 35320806 Free PMC article. No abstract available.
References
-
- Ikeda S., Yanai N., Ishikawa S. Flexible bronchofiberscope. Keio J Med. 1968;17(1):1–16. - PubMed
-
- Panchabhai T.S., Mehta A.C. Historical perspectives of bronchoscopy. Connecting the dots. Ann Am Thorac Soc. 2015;12(5):631–641. - PubMed
-
- Asano F., Shinagawa N., Ishida T., et al. Virtual bronchoscopic navigation combined with ultrathin bronchoscopy. A randomized clinical trial. Am J Respir Crit Care Med. 2013;188(3):327–333. - PubMed
-
- Eberhardt R., Anantham D., Ernst A., Feller-Kopman D., Herth F. Multimodality bronchoscopic diagnosis of peripheral lung lesions: a randomized controlled trial. Am J Respir Crit Care Med. 2007;176(1):36–41. - PubMed
-
- Folch E.E., Pritchett M.A., Nead M.A., et al. Electromagnetic navigation bronchoscopy for peripheral pulmonary lesions: one-year results of the prospective, multicenter NAVIGATE Study. J Thorac Oncol. 2019;14(3):445–458. - PubMed

