A pancancer overview of FBN1, asprosin and its cognate receptor OR4M1 with detailed expression profiling in ovarian cancer
- PMID: 34386072
- PMCID: PMC8298991
- DOI: 10.3892/ol.2021.12911
A pancancer overview of FBN1, asprosin and its cognate receptor OR4M1 with detailed expression profiling in ovarian cancer
Abstract
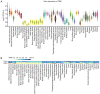
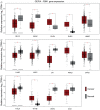
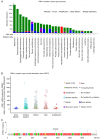
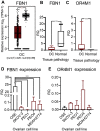
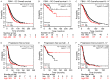
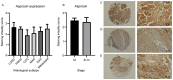
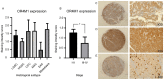
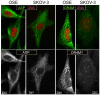
Ovarian cancer affects >295,000 women worldwide and is the most lethal of gynaecological malignancies. Often diagnosed at a late stage, current research efforts seek to further the molecular understanding of its aetiopathogenesis and the development of novel biomarkers. The present study investigated the expression levels of the glucogenic hormone asprosin [encoded by fibrillin-1 (FBN1)], and its cognate receptor, olfactory receptor 4M1 (OR4M1), in ovarian cancer. A blend of in silico open access The Cancer Genome Atlas data, as well as in vitro reverse transcription-quantitative PCR (RT-qPCR), immunohistochemistry and immunofluorescence data were used. RT-qPCR revealed expression levels of OR4M1 and FBN1 in clinical samples and in ovarian cancer cell lines (SKOV-3, PEO1, PEO4 and MDAH-2774), as well as the normal human ovarian surface epithelial cell line (HOSEpiC). Immunohistochemical staining of a tissue microarray was used to identify the expression levels of OR4M1 and asprosin in ovarian cancer samples of varying histological subtype and grade, including clear cell carcinoma, serous ovarian cancer and mucinous adenocarcinoma. Immunofluorescence analysis revealed asprosin expression in SKOV-3 and HOSEpiC cells. These results demonstrated the expression of both asprosin and OR4M1 in normal and malignant human ovarian tissues. This research invokes further investigation to advance the understanding of the role of asprosin and OR4M1 within the ovarian tumour microenvironment.
Keywords: asprosin; cancer; fibrillin-1; olfactory receptor; olfactory receptor 4M1; ovarian cancer.
Copyright: © Kerslake et al.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
Asprosin, a C-Terminal Cleavage Product of Fibrillin 1 Encoded by the FBN1 Gene, in Health and Disease.Mol Syndromol. 2022 May;13(3):175-183. doi: 10.1159/000520333. Epub 2022 Feb 8. Mol Syndromol. 2022. PMID: 35707591 Free PMC article. Review.
-
Developmental and hormonal regulation of FBN1 and OR4M1 mRNA in bovine granulosa cells.Domest Anim Endocrinol. 2023 Jul-Oct;84-85:106791. doi: 10.1016/j.domaniend.2023.106791. Epub 2023 Apr 25. Domest Anim Endocrinol. 2023. PMID: 37167929 Free PMC article.
-
Discovery of a possible role of asprosin in ovarian follicular function.J Mol Endocrinol. 2021 Jan;66(1):35-44. doi: 10.1530/JME-20-0218. J Mol Endocrinol. 2021. PMID: 33112803
-
Differential Regulation of Genes by the Glucogenic Hormone Asprosin in Ovarian Cancer.J Clin Med. 2022 Oct 8;11(19):5942. doi: 10.3390/jcm11195942. J Clin Med. 2022. PMID: 36233808 Free PMC article.
-
Energy Regulation Mechanism and Therapeutic Potential of Asprosin.Diabetes. 2020 Apr;69(4):559-566. doi: 10.2337/dbi19-0009. Diabetes. 2020. PMID: 32198197 Free PMC article. Review.
Cited by
-
Integrative, In Silico and Comparative Analysis of Breast Cancer Secretome Highlights Invasive-Ductal-Carcinoma-Grade Progression Biomarkers.Cancers (Basel). 2022 Aug 9;14(16):3854. doi: 10.3390/cancers14163854. Cancers (Basel). 2022. PMID: 36010848 Free PMC article.
-
Asprosin in health and disease, a new glucose sensor with central and peripheral metabolic effects.Front Endocrinol (Lausanne). 2023 Jan 5;13:1101091. doi: 10.3389/fendo.2022.1101091. eCollection 2022. Front Endocrinol (Lausanne). 2023. PMID: 36686442 Free PMC article. Review.
-
Elevated Circulating Lactate Levels and Widespread Expression of Its Cognate Receptor, Hydroxycarboxylic Acid Receptor 1 (HCAR1), in Ovarian Cancer.J Clin Med. 2022 Dec 27;12(1):217. doi: 10.3390/jcm12010217. J Clin Med. 2022. PMID: 36615018 Free PMC article.
-
Asprosin, a C-Terminal Cleavage Product of Fibrillin 1 Encoded by the FBN1 Gene, in Health and Disease.Mol Syndromol. 2022 May;13(3):175-183. doi: 10.1159/000520333. Epub 2022 Feb 8. Mol Syndromol. 2022. PMID: 35707591 Free PMC article. Review.
-
The Role of Meteorin-Like Peptide and Asprosin in Colon Carcinoma.Cureus. 2023 Oct 15;15(10):e47073. doi: 10.7759/cureus.47073. eCollection 2023 Oct. Cureus. 2023. PMID: 37846349 Free PMC article.
References
-
- Wang Y, Qu H, Xiong X, Qiu Y, Liao Y, Chen Y, Zheng Y, Zheng H. Plasma Asprosin Concentrations Are Increased in Individuals with Glucose Dysregulation and Correlated with Insulin Resistance and First-Phase Insulin Secretion. Mediators Inflamm. 2018;2018:9471583. doi: 10.1155/2018/9471583. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
