Donor genetic variants in interleukin-6 and interleukin-6 receptor associate with biopsy-proven rejection following kidney transplantation
- PMID: 34389747
- PMCID: PMC8363661
- DOI: 10.1038/s41598-021-95714-z
Donor genetic variants in interleukin-6 and interleukin-6 receptor associate with biopsy-proven rejection following kidney transplantation
Abstract
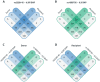
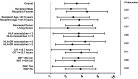
Rejection after kidney transplantation remains an important cause of allograft failure that markedly impacts morbidity. Cytokines are a major player in rejection, and we, therefore, explored the impact of interleukin-6 (IL6) and IL-6 receptor (IL6R) gene polymorphisms on the occurrence of rejection after renal transplantation. We performed an observational cohort study analyzing both donor and recipient DNA in 1271 renal transplant-pairs from the University Medical Center Groningen in The Netherlands and associated single nucleotide polymorphisms (SNPs) with biopsy-proven rejection after kidney transplantation. The C-allele of the IL6R SNP (Asp358Ala; rs2228145 A > C, formerly rs8192284) in donor kidneys conferred a reduced risk of rejection following renal transplantation (HR 0.78 per C-allele; 95%-CI 0.67-0.90; P = 0.001). On the other hand, the C-allele of the IL6 SNP (at position-174 in the promoter; rs1800795 G > C) in donor kidneys was associated with an increased risk of rejection for male organ donors (HR per C-allele 1.31; 95%-CI 1.08-1.58; P = 0.0006), but not female organ donors (P = 0.33). In contrast, neither the IL6 nor IL6R SNP in the recipient showed an association with renal transplant rejection. In conclusion, donor IL6 and IL6R genotypes but not recipient genotypes represent an independent prognostic marker for biopsy-proven renal allograft rejection.
© 2021. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures




Similar articles
-
Influence of recipient and donor IL-10, TNFA and INFG genotypes on the incidence of acute renal allograft rejection.Mol Biol Rep. 2009 Jul;36(6):1621-6. doi: 10.1007/s11033-008-9361-x. Epub 2008 Sep 16. Mol Biol Rep. 2009. PMID: 18792803
-
Association Between Cytokines and Their Receptor Antagonist Gene Polymorphisms and Clinical Risk Factors and Acute Rejection Following Renal Transplantation.Med Sci Monit. 2016 Dec 3;22:4736-4741. doi: 10.12659/msm.898193. Med Sci Monit. 2016. PMID: 27913812 Free PMC article.
-
Study of the cytokine polymorphisms in correlation to rejection and graft survival in renal allograft donors and recipients from a homogenous Saudi population.Transpl Immunol. 2014 Jan;30(1):34-9. doi: 10.1016/j.trim.2013.11.006. Epub 2013 Dec 4. Transpl Immunol. 2014. PMID: 24316141
-
Association between IL-6 -174G/C polymorphism and acute rejection of renal allograft: evidence from a meta-analysis.Transpl Immunol. 2012 Jan;26(1):11-8. doi: 10.1016/j.trim.2011.10.003. Epub 2011 Oct 17. Transpl Immunol. 2012. PMID: 22024650 Review.
-
Donor or recipient TNF-A -308G/A polymorphism and acute rejection of renal allograft: A meta-analysis.Transpl Immunol. 2011 Jul;25(1):61-71. doi: 10.1016/j.trim.2011.04.004. Epub 2011 May 7. Transpl Immunol. 2011. PMID: 21586325 Review.
Cited by
-
Association Between Pre-Transplant Oral Health and Post-Liver Transplant Complications.Transpl Int. 2023 Sep 12;36:11534. doi: 10.3389/ti.2023.11534. eCollection 2023. Transpl Int. 2023. PMID: 37767526 Free PMC article.
-
A non-muscle myosin heavy chain 9 genetic variant is associated with graft failure following kidney transplantation.Kidney Res Clin Pract. 2023 May;42(3):389-402. doi: 10.23876/j.krcp.22.061. Epub 2023 May 22. Kidney Res Clin Pract. 2023. PMID: 37313613 Free PMC article.
-
Donor and Recipient Polygenic Risk Scores Influence Kidney Transplant Function.Transpl Int. 2025 Mar 4;38:14171. doi: 10.3389/ti.2025.14171. eCollection 2025. Transpl Int. 2025. PMID: 40104404 Free PMC article.
-
An interleukin 6-based genetic risk score strengthened with interleukin 10 polymorphisms associated with long-term kidney allograft outcomes.Am J Transplant. 2022 Dec;22 Suppl 4(Suppl 4):45-57. doi: 10.1111/ajt.17212. Am J Transplant. 2022. PMID: 36453708 Free PMC article.
-
Crosstalk mechanisms between glomerular endothelial cells and podocytes in renal diseases and kidney transplantation.Kidney Res Clin Pract. 2024 Jan;43(1):47-62. doi: 10.23876/j.krcp.23.071. Epub 2023 Dec 8. Kidney Res Clin Pract. 2024. PMID: 38062623 Free PMC article.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

