Magnetic Resonance Imaging of Blood-Brain Barrier permeability in Dementia
- PMID: 34400249
- PMCID: PMC8528227
- DOI: 10.1016/j.neuroscience.2021.08.003
Magnetic Resonance Imaging of Blood-Brain Barrier permeability in Dementia
Abstract
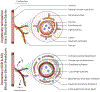
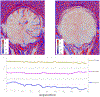
Alzheimer's disease (AD) and cerebral small vessel disease (cSVD) are the two main causes of dementia with blood-brain barrier (BBB) breakdown being a common contributor. Recent advances in neuroimaging techniques offer new possibilities to understand how the brain functions in health and disease. This includes methods such as dynamic contrast-enhanced magnetic resonance imaging (DCE-MRI) which allows the detection of subtle regional changes in the BBB integrity. The purpose of this work is to provide a review on the recent DCE-MRI findings of subtle BBB leakage focusing on cSVD and AD, including both clinical and pre-clinical studies. Despite being widely used and well-established, we also highlight some of the DCE-MRI challenges and pitfalls faced in the context of dementia inherent to the subtle nature of BBB impairment.
Keywords: Alzheimer's disease; blood-brain barrier; cerebral small vessel disease; dementia; magnetic resonance imaging.
Copyright © 2021 IBRO. Published by Elsevier Ltd. All rights reserved.
Figures
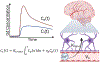

References
-
- Abbott NJ, Patabendige AAK, Dolman DEM, Yusof SR, Begley DJ (2010) Structure and function of the blood-brain barrier. Neurobiol Dis 37:13–25. - PubMed
-
- Baloyannis SJ, Baloyannis IS (2012) The vascular factor in Alzheimer’s disease: a study in Golgi technique and electron microscopy. J Neurol Sci 322:117–121. - PubMed
-
- Begley DJ, Brightman MW (2003) Structural and functional aspects of the blood-brain barrier. Prog Drug Res Fortschritte Arzneimittelforschung Progres Rech Pharm 61:39–78. - PubMed
-
- Bernal J, Valdés-Hernández M d. C, Escudero J, Heye AK, Sakka E, Armitage PA, Makin S, Touyz RM, Wardlaw JM, Thrippleton MJ (2021) A four-dimensional computational model of dynamic contrast-enhanced magnetic resonance imaging measurement of subtle blood-brain barrier leakage. NeuroImage 230:117786. - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

