Recovery and Prediction of Bimanual Hand Use After Stroke
- PMID: 34400568
- PMCID: PMC8377875
- DOI: 10.1212/WNL.0000000000012366
Recovery and Prediction of Bimanual Hand Use After Stroke
Erratum in
-
Recovery and Prediction of Bimanual Hand Use After Stroke.Neurology. 2022 Feb 22;98(8):341. doi: 10.1212/WNL.0000000000012717. Epub 2021 Aug 31. Neurology. 2022. PMID: 34465631 Free PMC article. No abstract available.
Abstract
Objective: To determine similarities and differences in key predictors of recovery of bimanual hand use and unimanual motor impairment after stroke.
Method: In this prospective longitudinal study, 89 patients with first-ever stroke with arm paresis were assessed at 3 weeks and 3 and 6 months after stroke onset. Bimanual activity performance was assessed with the Adult Assisting Hand Assessment Stroke (Ad-AHA), and unimanual motor impairment was assessed with the Fugl-Meyer Assessment (FMA). Candidate predictors included shoulder abduction and finger extension measured by the corresponding FMA items (FMA-SAFE; range 0-4) and sensory and cognitive impairment. MRI was used to measure weighted corticospinal tract lesion load (wCST-LL) and resting-state interhemispheric functional connectivity (FC).
Results: Initial Ad-AHA performance was poor but improved over time in all (mild-severe) impairment subgroups. Ad-AHA correlated with FMA at each time point (r > 0.88, p < 0.001), and recovery trajectories were similar. In patients with moderate to severe initial FMA, FMA-SAFE score was the strongest predictor of Ad-AHA outcome (R 2 = 0.81) and degree of recovery (R 2 = 0.64). Two-point discrimination explained additional variance in Ad-AHA outcome (R 2 = 0.05). Repeated analyses without FMA-SAFE score identified wCST-LL and cognitive impairment as additional predictors. A wCST-LL >5.5 cm3 strongly predicted low to minimal FMA/Ad-AHA recovery (≤10 and 20 points respectively, specificity = 0.91). FC explained some additional variance to FMA-SAFE score only in unimanual recovery.
Conclusion: Although recovery of bimanual activity depends on the extent of corticospinal tract injury and initial sensory and cognitive impairments, FMA-SAFE score captures most of the variance explained by these mechanisms. FMA-SAFE score, a straightforward clinical measure, strongly predicts bimanual recovery.
Clinicaltrialsgov identifier: NCT02878304.
Classification of evidence: This study provides Class I evidence that the FMA-SAFE score predicts bimanual recovery after stroke.
Copyright © 2021 The Author(s). Published by Wolters Kluwer Health, Inc. on behalf of the American Academy of Neurology.
Figures
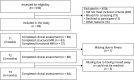



References
-
- Mayo NE, Wood-Dauphinee S, Cote R, Durcan L, Carlton J. Activity, participation, and quality of life 6 months poststroke. Arch Phys Med Rehabil. 2002;83(8):1035-1042. - PubMed
-
- Wu CY, Chou SH, Chen CL, Kuo MY, Lu TW, Fu YC. Kinematic analysis of a functional and sequential bimanual task in patients with left hemiparesis: intra-limb and interlimb coordination. Disabil Rehabil 2009;31:958-966. - PubMed
-
- Lodha N, Coombes SA, Cauraugh JH. Bimanual isometric force control: asymmetry and coordination evidence post stroke. Clin Neurophysiol. 2012;123:787-795. - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials
