Propofol Ameliorates Exaggerated Human Neutrophil Activation in a LPS Sepsis Model
- PMID: 34408467
- PMCID: PMC8366786
- DOI: 10.2147/JIR.S314192
Propofol Ameliorates Exaggerated Human Neutrophil Activation in a LPS Sepsis Model
Abstract
Background: Sepsis is a leading cause of morbidity and mortality worldwide. Many patients suffering from sepsis are treated on intensive care units and many of them require mechanical ventilation under sedation or general anesthesia. Propofol, a drug used for these purposes, is known to interact with polymorphonuclear granulocytes (PMNs). Therefore, the aim of this study was to investigate the influence of propofol on PMN functions after experimental Gram-negative induced sepsis using lipopolysaccharide (LPS) stimulation.
Methods: A total of 34 granulocyte-enriched samples were collected from healthy subjects. PMNs were isolated by density gradient centrifugation and incubated simultaneously with either 6 µg/mL or 60 µg/mL propofol, or none (control). Additionally, the experimental sepsis samples were incubated with either 40 pg/mL or 400 pg/mL LPS. Live cell imaging was conducted in order to observe granulocyte chemotactic migration, ROS production, and NETosis. Flow cytometry was used to analyze viability and antigen expression.
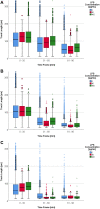
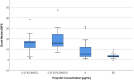
Results: Propofol led to significantly reduced PMN track length (p < 0.001) and track speed (p < 0.014) after LPS-induced sepsis in a dose-dependent manner. NETosis (p = 0.018) and ROS production (p = 0.039) were accelerated by propofol without LPS incubation, indicating improved immune function. Propofol also ameliorated LPS-induced increased NETosis and ROS-production. Antigen expression for CD11b, CD62l and CD66b was unaffected by propofol.
Conclusion: Propofol improves LPS-induced exaggerated PMN activation in an ex vivo model. Beneficial effects due to restored immune function in septic patients might be possible, but needs further investigation.
Keywords: LPS; immune modulation; polymorphonuclear neutrophils; propofol; sepsis.
© 2021 Bredthauer et al.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


References
LinkOut - more resources
Full Text Sources
Research Materials

