Impact of COVID-19 Infection on the Outcome of Patients With Ischemic Stroke
- PMID: 34455823
- PMCID: PMC8607902
- DOI: 10.1161/STROKEAHA.121.034883
Impact of COVID-19 Infection on the Outcome of Patients With Ischemic Stroke
Abstract
Background and purpose: We evaluated whether stroke severity, functional outcome, and mortality are different in patients with ischemic stroke with or without coronavirus disease 2019 (COVID-19) infection.
Methods: A prospective, observational, multicentre cohort study in Catalonia, Spain. Recruitment was consecutive from mid-March to mid-May 2020. Patients had an acute ischemic stroke within 48 hours and a previous modified Rankin Scale (mRS) score of 0 to 3. We collected demographic data, vascular risk factors, prior mRS score, National Institutes of Health Stroke Scale score, rate of reperfusion therapies, logistics, and metrics. Primary end point was functional outcome at 3 months. Favourable outcome was defined depending on the previous mRS score. Secondary outcome was mortality at 3 months. We performed mRS shift and multivariable analyses.
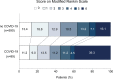
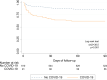
Results: We evaluated 701 patients (mean age 72.3±13.3 years, 60.5% men) and 91 (13%) had COVID-19 infection. Median baseline National Institutes of Health Stroke Scale score was higher in patients with COVID-19 compared with patients without COVID-19 (8 [3-18] versus 6 [2-14], P=0.049). Proportion of patients with a favourable functional outcome was 33.7% in the COVID-19 and 47% in the non-COVID-19 group. However, after a multivariable logistic regression analysis, COVID-19 infection did not increase the probability of unfavourable functional outcome. Mortality rate was 39.3% among patients with COVID-19 and 16.1% in the non-COVID-19 group. In the multivariable logistic regression analysis, COVID-19 infection was a risk factor for mortality (hazard ratio, 3.14 [95% CI, 2.10-4.71]; P<0.001).
Conclusions: Patients with ischemic stroke and COVID-19 infection have more severe strokes and a higher mortality than patients with stroke without COVID-19 infection. However, functional outcome is comparable in both groups.
Keywords: cerebrovascular disease; coronavirus; pandemics; prognosis; reperfusion; stroke; thrombectomy.
Figures
References
-
- Wu Z, McGoogan JM. Characteristics of and important lessons from the Coronavirus Disease 2019 (COVID-19) Outbreak in China: summary of a report of 72 314 cases Ffrom the Chinese Center for Disease Control and Prevention. JAMA. 2020;323:1239–1242. doi: 10.1001/jama.2020.2648 - PubMed
-
- Richardson S, Hirsch JS, Narasimhan M, Crawford JM, McGinn T, Davidson KW, Barnaby DP, Becker LB, Chelico JD, Cohen SL, et al. ; the Northwell COVID-19 Research Consortium. Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized With COVID-19 in the New York City Area. JAMA. 2020;323:2052–2059. doi: 10.1001/jama.2020.6775 - PMC - PubMed
-
- Cummings MJ, Baldwin MR, Abrams D, Jacobson SD, Meyer BJ, Balough EM, Aaron JG, Claassen J, Rabbani LE, Hastie J, et al. Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: a prospective cohort study. Lancet. 2020;395:1763–1770. doi: 10.1016/S0140-6736(20)31189-2 - PMC - PubMed
-
- Romero-Sánchez CM, Díaz-Maroto I, Fernández-Díaz E, Sánchez-Larsen Á, Layos-Romero A, García-García J, González E, Redondo-Peñas I, Perona-Moratalla AB, Del Valle-Pérez JA, et al. Neurologic manifestations in hospitalized patients with COVID-19: The ALBACOVID registry. Neurology. 2020;95:e1060–e1070. doi: 10.1212/WNL.0000000000009937 - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical