Bilateral Hypertrophic Olivary Degeneration Following Brainstem Insult: A Retrospective Review and Examination of Causative Pathology
- PMID: 34485912
- PMCID: PMC8415640
- DOI: 10.1177/26331055211007445
Bilateral Hypertrophic Olivary Degeneration Following Brainstem Insult: A Retrospective Review and Examination of Causative Pathology
Abstract
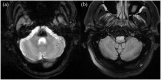
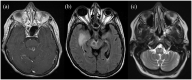
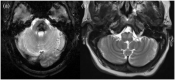
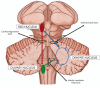
Hypertrophic olivary degeneration is a rare condition caused by a lesion in the Guillain-Mollaret triangle which leads to trans-synaptic degeneration resulting in the degenerative hypertrophy of the inferior olivary nucleus. This condition presents clinically with palatal tremor but can also produce ocular myoclonus or cerebellar signs. While any lesion that occurs within the Guillian-Mollaret triangle and results in the deafferentation of the inferior olive can lead to hypertrophic olivary degeneration, the most common etiologies include ischemic and hemorrhagic stroke, vascular malformation, neoplasm, and iatrogenic injury related to surgery. We report a series of 7 patients who presented with this condition bilaterally on MRI imaging, including 1 case which represents the first report of toxoplasmosis leading to the development of bilateral hypertrophic olivary degeneration and only the third reported case, unilateral or bilateral, related to an infectious etiology.
Keywords: Guillain-Mollaret Triangle; Neuroanatomy; hypertrophic olivary degeneration; inferior olivary nucleus; palatal tremor.
© The Author(s) 2021.
Conflict of interest statement
Declaration of conflicting interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
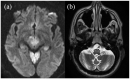
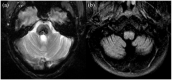
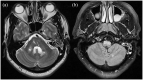
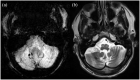
References
-
- Oppenheim H. Über Olivendegeneration bei Atheromatose der basalen Hirnarterien. Berl Klin Wochenschr. 1887;34:638-639.
-
- Gautier J, Blackwood W. Enlargement of the inferior olivary nucleus in association with lesions of the central tegmental tract or dentate nucleus. Brain. 1961;84:341-361. - PubMed
-
- Foix C, Chavany J, Hillemand P. Le Syndrome myoclonique de la calotte. Rev Neurol. 1926;33:942-956.
-
- Guillain G, Mollaret P. Deux cas de myoclonies synchrones et rythmées vélo-pliaryngo-oculo-diaphragmatiques. Le problème anatomique et physio-pathologique de ce syndrome. Rev Neurol. 1931;2:545-566.
-
- Bouz P, Woods ROJ, Woods KRM. The pathophysiological basis for hypertrophic olivary degeneration (HOD) following brainstem insult. JSM Neurosurg Spine. 2013;1:1004
Publication types
LinkOut - more resources
Full Text Sources

