Rectus Abdominis Flap Replantation after 18 h Hypothermic Extracorporeal Perfusion-A Porcine Model
- PMID: 34501304
- PMCID: PMC8432231
- DOI: 10.3390/jcm10173858
Rectus Abdominis Flap Replantation after 18 h Hypothermic Extracorporeal Perfusion-A Porcine Model
Abstract
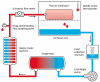
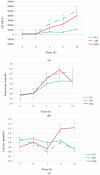
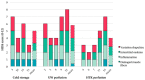
Cold storage remains the clinical standard for composite tissue preservation but is time-limited. A long ischemia time during surgery will adversely affect postoperative outcomes due to ischemia-reperfusion injury. Extracorporeal perfusion (ECP) seems to be a promising alternative for prolonged preservation, but more evidence is needed to support its use and to identify optimal perfusion fluids. This article assessed musculocutaneous flap vitality after prolonged ECP and compared outcomes after replantation to short static cold storage (SCS). Unilateral musculocutaneous rectus abdominis flaps were raised from 15 pigs and preserved by 4 h SCS (n = 5), 18 h mid-thermic ECP with Histidine-Tryptophan-Ketoglutarate (HTK, n = 5) or University of Wisconsin solution (UW, n = 5). Flaps were replanted and observed for 12 h. Skeletal muscle histology was assessed (score 0-12; high scores equal more damage), blood and perfusate samples were collected and weight was recorded as a marker for oedema. Mean histological scores were 4.0 after HTK preservation, 5.6 after UW perfusion and 5.0 after SCS (p = 0.366). Creatinine kinase (CK) was higher after ECP compared to SCS (p < 0.001). No weight increase was observed during UW perfusion, but increased 56% during HTK perfusion. Following 12 h reperfusion, mean weight gain reduced 39% in the HTK group and increased 24% in the UW group and 17% in the SCS group. To conclude, skeletal muscle seemed well preserved after 18 h ECP with HTK or UW perfusion, with comparable histological results to 4 h SCS upon short reperfusion. The high oedema rate during HTK perfusion remains a challenge that needs to be further addressed.
Keywords: VCA; composite tissue transplantation; ex vivo preservation; free flap; mid-thermic storage.
Conflict of interest statement
The authors declare no conflict of interest.
Figures



Similar articles
-
Successful Long-term Extracorporeal Perfusion of Free Musculocutaneous Flaps in a Porcine Model.J Surg Res. 2019 Mar;235:113-123. doi: 10.1016/j.jss.2018.09.076. Epub 2018 Oct 25. J Surg Res. 2019. PMID: 30691784
-
Successful 18-h acellular extracorporeal perfusion and replantation of porcine limbs - Histology versus nerve stimulation.Transpl Int. 2021 Feb;34(2):365-375. doi: 10.1111/tri.13802. Epub 2021 Jan 5. Transpl Int. 2021. PMID: 33316847 Free PMC article.
-
24-hour Perfusion of Porcine Myocutaneous Flaps Mitigates Reperfusion Injury: A 7-day Follow-up Study.Plast Reconstr Surg Glob Open. 2022 Feb 21;10(2):e4123. doi: 10.1097/GOX.0000000000004123. eCollection 2022 Feb. Plast Reconstr Surg Glob Open. 2022. PMID: 35211366 Free PMC article.
-
Influence of perfusate on liver viability during hypothermic machine perfusion.World J Gastroenterol. 2015 Aug 7;21(29):8848-57. doi: 10.3748/wjg.v21.i29.8848. World J Gastroenterol. 2015. PMID: 26269674 Free PMC article.
-
Review of machine perfusion studies in vascularized composite allotransplant preservation.Front Transplant. 2023 Dec 20;2:1323387. doi: 10.3389/frtra.2023.1323387. eCollection 2023. Front Transplant. 2023. PMID: 38993931 Free PMC article. Review.
Cited by
-
Sub-Zero Non-Freezing of Vascularized Composite Allografts Preservation in Rodents.Res Sq [Preprint]. 2023 Dec 25:rs.3.rs-3750450. doi: 10.21203/rs.3.rs-3750450/v1. Res Sq. 2023. Update in: Cryobiology. 2024 Sep;116:104950. doi: 10.1016/j.cryobiol.2024.104950. PMID: 38234765 Free PMC article. Updated. Preprint.
-
Enhancing Vascularized Composite Allograft Supercooling Preservation: A Multifaceted Approach with CPA Optimization, Thermal Tracking, and Stepwise Loading Techniques.Res Sq [Preprint]. 2024 Jun 11:rs.3.rs-4431685. doi: 10.21203/rs.3.rs-4431685/v1. Res Sq. 2024. Update in: Sci Rep. 2024 Sep 27;14(1):22339. doi: 10.1038/s41598-024-73549-8. PMID: 38946999 Free PMC article. Updated. Preprint.
-
Continuous versus Pulsatile Flow in 24-Hour Vascularized Composite Allograft Machine Perfusion in Swine: A Pilot Study.J Surg Res. 2023 Mar;283:1145-1153. doi: 10.1016/j.jss.2022.11.003. Epub 2022 Dec 16. J Surg Res. 2023. PMID: 36915006 Free PMC article.
-
Sub-zero non-freezing of vascularized composite allografts in a rodent partial hindlimb model.Cryobiology. 2024 Sep;116:104950. doi: 10.1016/j.cryobiol.2024.104950. Epub 2024 Aug 24. Cryobiology. 2024. PMID: 39134131
-
Effect of Subnormothermic Machine Perfusion on the Preservation of Vascularized Composite Allografts After Prolonged Warm Ischemia.Transplantation. 2024 Nov 1;108(11):2222-2232. doi: 10.1097/TP.0000000000005035. Epub 2024 Oct 22. Transplantation. 2024. PMID: 38722685
References
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

