Risk factors associated with intra-stent restenosis after percutaneous coronary intervention
- PMID: 34504587
- PMCID: PMC8394103
- DOI: 10.3892/etm.2021.10575
Risk factors associated with intra-stent restenosis after percutaneous coronary intervention
Abstract
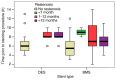
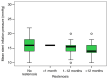
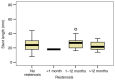
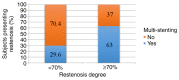
The present study aimed to explore the correlations between clinical, biological, imagistic and procedural factors with the risk of intra-stent restenosis (ISR) in coronary artery disease (CAD) patients after percutaneous coronary intervention (PCI). An observational cross-sectional study was conducted in a high-volume PCI center over a period of 2 years. A total of 235 consecutive patients diagnosed with angina or acute coronary syndrome treated by PCI were included in the study. Diagnosis of ISR was documented by coronary angiography in patients with suggestive coronary symptoms and ischemic changes in non-invasive or invasive paraclinical investigations. Thus, they were assigned to two groups: With or without ISR. All patients underwent clinical and laboratory examination, providing clinical and paraclinical variables that could be considered risk factors for ISR. Current smokers [risk ratio (RR)=1.63; 95% confidence interval (95% CI): 1.25-2.13], arterial hypertension (RR=1.86; 95% CI: 1.41-2.45), diabetes (RR=1.83; 95% CI: 1.42-2.36), high C-reactive protein (CRP) levels (RR=1.44; 95% CI: 0.93-2.24), chronic kidney disease (CKD) (RR=1.90; 95% CI: 1.53-2.36) and thrombolysis in myocardial infarction (TIMI) score were found to have a significant role in estimating the risk for ISR. Moreover, the ISR group (119 patients) presented with a lower stent inflation pressure when compared to the control group (116 patients) (14.47 vs. 16.14 mmHg, P=0.004). An increased mean stent diameter used for PCI was not associated with a high ISR incidence (P=0.810) as well as complex coronary treated lesions with longer stents (mean length of 24.98 mm in patients without ISR vs. 25.22 mm in patients with ISR; P=0.311). There was an estimated two times higher risk (RR=2.13; 95% CI: 1.17-3.88) concerning multi-stenting and restenosis degree >70%. To conclude, smoking, hypertension, diabetes mellitus, high CRP levels, CKD, TIMI score, stent type, low pressure for stent implantation and multi-stenting were found to be associated with ISR in patients following PCI. Therefore, a close follow-up should be targeted in such patients.
Keywords: BMS; DES; coronary artery disease; percutaneous coronary intervention; risk factors; stent restenosis.
Copyright: © Alexandrescu et al.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

References
-
- Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, Abraham J, Adair T, Aggarwal R, Ahn SY, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: A systematic analysis for the global burden of disease study. Lancet. 2012;380:2095–2128. doi: 10.1016/S0140-6736(12)61728-0. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
