Risk Factors for HIV sero-conversion in a high incidence cohort of men who have sex with men and transgender women in Bangkok, Thailand
- PMID: 34505031
- PMCID: PMC8413240
- DOI: 10.1016/j.eclinm.2021.101033
Risk Factors for HIV sero-conversion in a high incidence cohort of men who have sex with men and transgender women in Bangkok, Thailand
Abstract
Background: We measured Human Immunodeficiency (HIV) incidence, retention, and assessed risk factors for seroconversion among two previously unreported cohorts of men who have sex with men (MSM) and Transgender Women (TGW) in Bangkok, Thailand between 2017 and 2019.
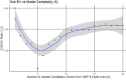
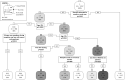
Methods: We conducted an 18-month prospective cohort study of HIV-uninfected Thai cisgender men and TGW aged between 18 and 35 years who reported sex with men in the past six months and at least one additional risk factor for HIV infection. HIV and syphilis testing and computer-based behavioral questionnaires were administered at each visit. We utilized Poisson regression to calculate HIV incidence rates. A survival random forest model identified the most predictive risk factors for HIV sero-conversion and then used in a survival regression tree model to elucidate hazard ratios for individuals with groups of selected risk factors. Cox proportional hazards (pH) regression evaluated the strength of association between individual covariates and risk of sero-conversion.
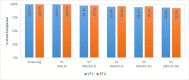
Findings: From April 2017-October 2019, 1,184 participants were screened, 167 were found ineligible, and 1,017 enrolled. Over the 18-month study, visit retention was 93·4% (95% CI 91·6%-94·8%) and HIV incidence was 3·73 per 100 person-years (95% CI 2·79-5·87). Utilizing survival regression tree modeling, those who were 18-20 years of age, reported sexual attraction to mostly or only men, and had five or more lifetime sexual partners were 4·9 times more likely to seroconvert compared to other cohort participants. Factors associated with HIV incidence utilizing Cox pH regression included sexual attraction to mostly or only men (adjusted hazard ratio (aHR) 14·9 (95% CI 20·1-107·9), younger age (18-19 years, aHR 10·88 (95% CI 4·12-28·7), five or greater lifetime sexual partners (aHR 2·0, 95%CI 1·1-3·6), inconsistent condom use with casual partners (aHR 2·43, 95% CI 1·3-4·5), and prior HIV testing (adjusted HR 2·0, 95% CI 1·1-3·5).
Interpretation: Interpretation HIV incidence remains high among Bangkok-based MSM and TGW. These key populations expressed high interest in participating in efficacy evaluation of future prevention strategies and had high retention in this 18 month study.
Funding: Funding US National Institute of Allergy and Infectious Diseases (NIAID), Division of AIDS Interagency Agreements (DAIDS) and U.S. Department of the Army.
© 2021 Henry M. Jackson Foundation for the Advancement of Military Medicine.
Conflict of interest statement
None.
Figures





References
-
- TWGoHA Projection. Summary Report; 2010. AIDS Epidemic Model Projection for HIV/Aids in Thailand, 2010–2030.
-
- AIDS Zero Portal . 2019. Data Use Tool [Internet]https://hivhub.ddc.moph.go.th/ [cited July 20, 2020]. Available from:
-
- Thai Ministry of Public Health TAS . Department of Disease Control; 2017. Thailand National Guidelines on HIV/Aids Treatment and Prevention. Office of AIDS, TB, and STI, Thai Ministry of Public Health.
LinkOut - more resources
Full Text Sources
Miscellaneous

