Management of Spontaneous Bleeding in COVID-19 Inpatients: Is Embolization Always Needed?
- PMID: 34575230
- PMCID: PMC8469448
- DOI: 10.3390/jcm10184119
Management of Spontaneous Bleeding in COVID-19 Inpatients: Is Embolization Always Needed?
Abstract
Background: critically ill patients with SARS-CoV-2 infection present a hypercoagulable condition. Anticoagulant therapy is currently recommended to reduce thrombotic risk, leading to potentially severe complications like spontaneous bleeding (SB). Percutaneous transcatheter arterial embolization (PTAE) can be life-saving in critical patients, in addition to medical therapy. We report a major COVID-19 Italian Research Hospital experience during the pandemic, with particular focus on indications and technique of embolization.
Methods: We retrospectively included all subjects with SB and with a microbiologically confirmed SARS-CoV-2 infection, over one year of pandemic, selecting two different groups: (a) patients treated with PTAE and medical therapy; (b) patients treated only with medical therapy. Computed tomography (CT) scan findings, clinical conditions, and biological findings were collected.
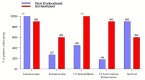
Results: 21/1075 patients presented soft tissue SB with an incidence of 1.95%. 10/21 patients were treated with PTAE and medical therapy with a 30-days survival of 70%. Arterial blush, contrast late enhancement, and dimensions at CT scan were found discriminating for the embolization (p < 0.05).
Conclusions: PTAE is an important tool in severely ill, bleeding COVID-19 patients. The decision for PTAE of COVID-19 patients must be carefully weighted with particular attention paid to the clinical and biological condition, hematoma location and volume.
Keywords: COVID-19; low-molecular-weight heparin; percutaneous trans arterial embolization; spontaneous bleeding.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures



References
-
- World Health Organization Coronavirus Disease 2019 (COVID-19) Situation Report—72. [(accessed on 1 April 2020)]. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/2....
-
- Zhou F., Yu T., Du R., Fan G., Liu Y., Liu Z., Xiang J., Wang Y., Song B., Gu X., et al. Clinical Course and Risk Factors for Mortality of Adult Inpatients with COVID-19 in Wuhan, China: A Retrospective Cohort Study. Lancet. 2020;395:1054–1062. doi: 10.1016/S0140-6736(20)30566-3. - DOI - PMC - PubMed
-
- Bikdeli B., Madhavan M.V., Jimenez D., Chuich T., Dreyfus I., Driggin E., Nigoghossian C.D., Ageno W., Madjid M., Guo Y., et al. COVID-19 and Thrombotic or Thromboembolic Disease: Implications for Prevention, Antithrombotic Therapy, and Follow-Up: JACC State-of-the-Art Review. J Am Coll Cardiol. 2020;75:2950–2973. doi: 10.1016/j.jacc.2020.04.031. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

