Burn Injury Induces Proinflammatory Plasma Extracellular Vesicles That Associate with Length of Hospital Stay in Women: CRP and SAA1 as Potential Prognostic Indicators
- PMID: 34576246
- PMCID: PMC8468249
- DOI: 10.3390/ijms221810083
Burn Injury Induces Proinflammatory Plasma Extracellular Vesicles That Associate with Length of Hospital Stay in Women: CRP and SAA1 as Potential Prognostic Indicators
Abstract
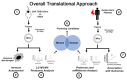
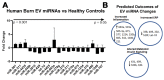
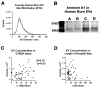
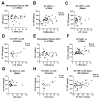
Severe burn injury is a devastating form of trauma that results in persistent immune dysfunction with associated morbidity and mortality. The underlying drivers of this immune dysfunction remain elusive, and there are no prognostic markers to identify at-risk patients. Extracellular vesicles (EVs) are emerging as drivers of immune dysfunction as well as biomarkers. We investigated if EVs after burn injury promote macrophage activation and assessed if EV contents can predict length of hospital stay. EVs isolated early from mice that received a 20% total body surface area (TBSA) burn promoted proinflammatory responses in cultured splenic macrophages. Unbiased LC-MS/MS proteomic analysis of early EVs (<72 h post-injury) from mice and humans showed some similarities including enrichment of acute phase response proteins such as CRP and SAA1. Semi-unbiased assessment of early human burn patient EVs found alterations consistent with increased proinflammatory signaling and loss of inhibition of CRP expression. In a sample of 50 patients with large burn injury, EV SAA1 and CRP were correlated with TBSA injury in both sexes and were correlated with length of hospital stay in women. These findings suggest that EVs are drivers of immune responses after burn injury and their content may predict hospital course.
Keywords: biomarkers; burn injury; extracellular vesicles; sepsis; trauma.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analysis, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures



References
-
- ABA National Burn Repository Burn Incidence and Treatment in the United States: 2016. [(accessed on 1 September 2021)]. Available online: http://ameriburn.org/resources_factsheet.php.
-
- Maile R., Jones S., Pan Y., Zhou H., Jaspers I., Peden D.B., Cairns B.A., Noah T.L. Association between early airway damage-associated molecular patterns and subsequent bacterial infection in patients with inhalational and burn injury. Am. J. Physiol. Lung Cell. Mol. Physiol. 2015;308:L855–L860. doi: 10.1152/ajplung.00321.2014. - DOI - PMC - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

