PUFA Supplementation and Heart Failure: Effects on Fibrosis and Cardiac Remodeling
- PMID: 34578843
- PMCID: PMC8471017
- DOI: 10.3390/nu13092965
PUFA Supplementation and Heart Failure: Effects on Fibrosis and Cardiac Remodeling
Abstract
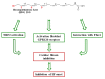
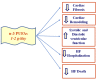
Heart failure (HF) characterized by cardiac remodeling is a condition in which inflammation and fibrosis play a key role. Dietary supplementation with n-3 polyunsaturated fatty acids (PUFAs) seems to produce good results. In fact, eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) have anti-inflammatory and antioxidant properties and different cardioprotective mechanisms. In particular, following their interaction with the nuclear factor erythropoietin 2 related factor 2 (NRF2), the free fatty acid receptor 4 (Ffar4) receptor, or the G-protein coupled receptor 120 (GPR120) fibroblast receptors, they inhibit cardiac fibrosis and protect the heart from HF onset. Furthermore, n-3 PUFAs increase the left ventricular ejection fraction (LVEF), reduce global longitudinal deformation, E/e ratio (early ventricular filling and early mitral annulus velocity), soluble interleukin-1 receptor-like 1 (sST2) and high-sensitive C Reactive protein (hsCRP) levels, and increase flow-mediated dilation. Moreover, lower levels of brain natriuretic peptide (BNP) and serum norepinephrine (sNE) are reported and have a positive effect on cardiac hemodynamics. In addition, they reduce cardiac remodeling and inflammation by protecting patients from HF onset after myocardial infarction (MI). The positive effects of PUFA supplementation are associated with treatment duration and a daily dosage of 1-2 g. Therefore, both the European Society of Cardiology (ESC) and the American College of Cardiology/American Heart Association (ACC/AHA) define dietary supplementation with n-3 PUFAs as an effective therapy for reducing the risk of hospitalization and death in HF patients. In this review, we seek to highlight the most recent studies related to the effect of PUFA supplementation in HF. For that purpose, a PubMed literature survey was conducted with a focus on various in vitro and in vivo studies and clinical trials from 2015 to 2021.
Keywords: HFpEF; HFrEF; PUFAs; cardiac fibrosis; cardiac remodeling; cardioprotective mechanism; heart failure; inflammation; myocardial infarction (MI).
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Chia N., Fulcher J., Keech A. Beta-blocker, angiotensin-converting enzyme inhibitor/angiotensin receptor blocker, nitrate-hydralazine, diuretics, aldosterone antagonist, ivabradine, devices and digoxin (BANDAID2): An evidence-based mnemonic for the treatment of systolic heart failure. Intern. Med. J. 2016;46:653–662. doi: 10.1111/imj.12839. - DOI - PubMed
-
- Mollace V., Rosano G.M.C., Anker S.D., Coats A.J.S., Seferovic P., Mollace R., Tavernese A., Gliozzi M., Musolino V., Carresi C., et al. Pathophysiological Basis for Nutraceutical Supplementation in Heart Failure: A Comprehensive Review. Nutrients. 2021;13:257. doi: 10.3390/nu13010257. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

