Gram-negative neonatal sepsis in low- and lower-middle-income countries and WHO empirical antibiotic recommendations: A systematic review and meta-analysis
- PMID: 34582466
- PMCID: PMC8478175
- DOI: 10.1371/journal.pmed.1003787
Gram-negative neonatal sepsis in low- and lower-middle-income countries and WHO empirical antibiotic recommendations: A systematic review and meta-analysis
Abstract
Background: Neonatal sepsis is a significant global health issue associated with marked regional disparities in mortality. Antimicrobial resistance (AMR) is a growing concern in Gram-negative organisms, which increasingly predominate in neonatal sepsis, and existing WHO empirical antibiotic recommendations may no longer be appropriate. Previous systematic reviews have been limited to specific low- and middle-income countries. We therefore completed a systematic review and meta-analysis of available data from all low- and lower-middle-income countries (LLMICs) since 2010, with a focus on regional differences in Gram-negative infections and AMR.
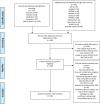
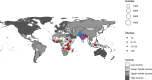
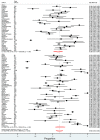
Methods and findings: All studies published from 1 January 2010 to 21 April 2021 about microbiologically confirmed bloodstream infections or meningitis in neonates and AMR in LLMICs were assessed for eligibility. Small case series, studies with a small number of Gram-negative isolates (<10), and studies with a majority of isolates prior to 2010 were excluded. Main outcomes were pooled proportions of Escherichia coli, Klebsiella, Enterobacter, Pseudomonas, Acinetobacter and AMR. We included 88 studies (4 cohort studies, 3 randomised controlled studies, and 81 cross-sectional studies) comprising 10,458 Gram-negative isolates from 19 LLMICs. No studies were identified outside of Africa and Asia. The estimated pooled proportion of neonatal sepsis caused by Gram-negative organisms was 60% (95% CI 55% to 65%). Klebsiella spp. was the most common, with a pooled proportion of 38% of Gram-negative sepsis (95% CI 33% to 43%). Regional differences were observed, with higher proportions of Acinetobacter spp. in Asia and Klebsiella spp. in Africa. Resistance to aminoglycosides and third-generation cephalosporins ranged from 42% to 69% and from 59% to 84%, respectively. Study limitations include significant heterogeneity among included studies, exclusion of upper-middle-income countries, and potential sampling bias, with the majority of studies from tertiary hospital settings, which may overestimate the burden caused by Gram-negative bacteria.
Conclusions: Gram-negative bacteria are an important cause of neonatal sepsis in LLMICs and are associated with significant rates of resistance to WHO-recommended first- and second-line empirical antibiotics. AMR surveillance should underpin region-specific empirical treatment recommendations. Meanwhile, a significant global commitment to accessible and effective antimicrobials for neonates is required.
Conflict of interest statement
I have read the journal’s policy and the authors of this manuscript have the following competing interests: SCW has previously received research grant from GSK. DLP has board memberships with Merck, Shionogi, Achaogen, AstraZeneca, Leo Pharmaceuticals, Bayer, GlaxoSmithKline, Cubist, Venatorx and Accelerate. DLP has received payment from Pfizer for lectures. DLP also has grants pending with Shinogi and Merck.
Figures

References
-
- World Health Organization. Reaching the Every Newborn national 2020 milestones: country progress, plans and moving forward. Geneva: World Health Organization; 2017.
-
- Investigators of the Delhi Neonatal Infection Study (DeNIS) collaboration. Characterisation and antimicrobial resistance of sepsis pathogens in neonates born in tertiary care centres in Delhi, India: a cohort study. Lancet Glob Health. 2016;4(10):e752–e60. doi: 10.1016/S2214-109X(16)30148-6 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

