Evaluation of the etiology and risk factors for maternal sepsis: A single center study in Guangzhou, China
- PMID: 34621821
- PMCID: PMC8462250
- DOI: 10.12998/wjcc.v9.i26.7704
Evaluation of the etiology and risk factors for maternal sepsis: A single center study in Guangzhou, China
Abstract
Background: Maternal sepsis is a major cause of gestational morbidity and neonatal mortality worldwide and particularly in China.
Aim: To evaluate the etiology of maternal sepsis and further identify its risk factors.
Methods: In this retrospective study, we evaluated 70698 obstetric patients who were admitted to the Third Affiliated Hospital of Guangzhou Medical University between January 1, 2009 and June 30, 2018. Subjects were divided into sepsis group and non-sepsis group based on the incidence of sepsis. Data about medical history (surgical and obstetric history) and demographic information were collected. The Mann-Whitney U test was used to compare patient age, gestational age and duration of hospitalization between the two groups. Univariate and multivariate logistic regression models were used to analyze the etiology and the risk factors for maternal sepsis. Unadjusted and adjusted odds ratios (OR) are reported.
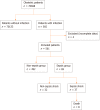
Results: A total of 561 of 70698 obstetric patients were diagnosed with infection; of the infected patients, 492 had non-sepsis associated infection (87.7%), while 69 had sepsis (12.3%). The morbidity rate of maternal sepsis was 9.76/10000; the fatality rate in the sepsis group was 11.6% (8/69). Emergency admission (OR = 2.183) or transfer (OR = 2.870), irregular prenatal care (OR = 2.953), labor induction (OR = 4.665), cervical cerclage (OR = 14.214), first trimester (OR = 6.806) and second trimester (OR = 2.09) were significant risk factors for maternal sepsis.
Conclusion: Mode of admission, poor prenatal care, labor induction, cervical cerclage, first trimester and second trimester pregnancy were risk factors for maternal sepsis. Escherichia coli was the most common causative organism for maternal sepsis, and the uterus was the most common site of infection.
Keywords: Infection; Maternal sepsis; Risk factors; Sepsis-3.
©The Author(s) 2021. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors declare that they have no conflict of interest.
Figures
Similar articles
-
[Clinical analysis of 68 cases of sepsis during pregnancy and the postpartum period].Zhonghua Fu Chan Ke Za Zhi. 2020 Nov 25;55(11):770-777. doi: 10.3760/cma.j.cn112141-20200521-00430. Zhonghua Fu Chan Ke Za Zhi. 2020. PMID: 33228348 Chinese.
-
Association of abnormal first stage of labor duration and maternal and neonatal morbidity.Am J Obstet Gynecol. 2020 Sep;223(3):445.e1-445.e15. doi: 10.1016/j.ajog.2020.06.053. Am J Obstet Gynecol. 2020. PMID: 32883453
-
[Analysis of clinical effect of McDonald cervical cerclage and the related risk factors].Zhonghua Fu Chan Ke Za Zhi. 2016 Feb;51(2):87-91. doi: 10.3760/cma.j.issn.0529-567X.2016.02.002. Zhonghua Fu Chan Ke Za Zhi. 2016. PMID: 26917475 Chinese.
-
Maternal sepsis incidence, aetiology and outcome for mother and fetus: a prospective study.BJOG. 2015 Apr;122(5):663-71. doi: 10.1111/1471-0528.12892. Epub 2014 May 23. BJOG. 2015. PMID: 24862293 Review.
-
Maternal sepsis: background, diagnosis and management.BJA Educ. 2024 Nov;24(11):389-398. doi: 10.1016/j.bjae.2024.06.004. Epub 2024 Aug 13. BJA Educ. 2024. PMID: 39620103 Review. No abstract available.
Cited by
-
Evaluation of microbiological epidemiology and clinical characteristics of maternal bloodstream infection: a 10 years retrospective study.Front Microbiol. 2024 Jan 8;14:1332611. doi: 10.3389/fmicb.2023.1332611. eCollection 2023. Front Microbiol. 2024. PMID: 38264486 Free PMC article.
-
Double-blind, randomised, placebo-controlled trial to evaluate the effectiveness of late gestation oral melatonin supplementation in reducing induction of labour rates in nulliparous women: the MyTIME study protocol.BMJ Open. 2025 Jan 23;15(1):e090370. doi: 10.1136/bmjopen-2024-090370. BMJ Open. 2025. PMID: 39855663 Free PMC article.
-
Factors Associated with Increased Risk of Urosepsis during Pregnancy and Treatment Outcomes, in a Urology Clinic.Medicina (Kaunas). 2023 Nov 8;59(11):1972. doi: 10.3390/medicina59111972. Medicina (Kaunas). 2023. PMID: 38004021 Free PMC article.
References
-
- Kassebaum NJ, Bertozzi-Villa A, Coggeshall MS, Shackelford KA, Steiner C, Heuton KR, Gonzalez-Medina D, Barber R, Huynh C, Dicker D, Templin T, Wolock TM, Ozgoren AA, Abd-Allah F, Abera SF, Abubakar I, Achoki T, Adelekan A, Ademi Z, Adou AK, Adsuar JC, Agardh EE, Akena D, Alasfoor D, Alemu ZA, Alfonso-Cristancho R, Alhabib S, Ali R, Al Kahbouri MJ, Alla F, Allen PJ, AlMazroa MA, Alsharif U, Alvarez E, Alvis-Guzmán N, Amankwaa AA, Amare AT, Amini H, Ammar W, Antonio CA, Anwari P, Arnlöv J, Arsenijevic VS, Artaman A, Asad MM, Asghar RJ, Assadi R, Atkins LS, Badawi A, Balakrishnan K, Basu A, Basu S, Beardsley J, Bedi N, Bekele T, Bell ML, Bernabe E, Beyene TJ, Bhutta Z, Bin Abdulhak A, Blore JD, Basara BB, Bose D, Breitborde N, Cárdenas R, Castañeda-Orjuela CA, Castro RE, Catalá-López F, Cavlin A, Chang JC, Che X, Christophi CA, Chugh SS, Cirillo M, Colquhoun SM, Cooper LT, Cooper C, da Costa Leite I, Dandona L, Dandona R, Davis A, Dayama A, Degenhardt L, De Leo D, del Pozo-Cruz B, Deribe K, Dessalegn M, deVeber GA, Dharmaratne SD, Dilmen U, Ding EL, Dorrington RE, Driscoll TR, Ermakov SP, Esteghamati A, Faraon EJ, Farzadfar F, Felicio MM, Fereshtehnejad SM, de Lima GM, Forouzanfar MH, França EB, Gaffikin L, Gambashidze K, Gankpé FG, Garcia AC, Geleijnse JM, Gibney KB, Giroud M, Glaser EL, Goginashvili K, Gona P, González-Castell D, Goto A, Gouda HN, Gugnani HC, Gupta R, Hafezi-Nejad N, Hamadeh RR, Hammami M, Hankey GJ, Harb HL, Havmoeller R, Hay SI, Pi IB, Hoek HW, Hosgood HD, Hoy DG, Husseini A, Idrisov BT, Innos K, Inoue M, Jacobsen KH, Jahangir E, Jee SH, Jensen PN, Jha V, Jiang G, Jonas JB, Juel K, Kabagambe EK, Kan H, Karam NE, Karch A, Karema CK, Kaul A, Kawakami N, Kazanjan K, Kazi DS, Kemp AH, Kengne AP, Kereselidze M, Khader YS, Khalifa SE, Khan EA, Khang YH, Knibbs L, Kokubo Y, Kosen S, Defo BK, Kulkarni C, Kulkarni VS, Kumar GA, Kumar K, Kumar RB, Kwan G, Lai T, Lalloo R, Lam H, Lansingh VC, Larsson A, Lee JT, Leigh J, Leinsalu M, Leung R, Li X, Li Y, Liang J, Liang X, Lim SS, Lin HH, Lipshultz SE, Liu S, Liu Y, Lloyd BK, London SJ, Lotufo PA, Ma J, Ma S, Machado VM, Mainoo NK, Majdan M, Mapoma CC, Marcenes W, Marzan MB, Mason-Jones AJ, Mehndiratta MM, Mejia-Rodriguez F, Memish ZA, Mendoza W, Miller TR, Mills EJ, Mokdad AH, Mola GL, Monasta L, de la Cruz Monis J, Hernandez JC, Moore AR, Moradi-Lakeh M, Mori R, Mueller UO, Mukaigawara M, Naheed A, Naidoo KS, Nand D, Nangia V, Nash D, Nejjari C, Nelson RG, Neupane SP, Newton CR, Ng M, Nieuwenhuijsen MJ, Nisar MI, Nolte S, Norheim OF, Nyakarahuka L, Oh IH, Ohkubo T, Olusanya BO, Omer SB, Opio JN, Orisakwe OE, Pandian JD, Papachristou C, Park JH, Caicedo AJ, Patten SB, Paul VK, Pavlin BI, Pearce N, Pereira DM, Pesudovs K, Petzold M, Poenaru D, Polanczyk GV, Polinder S, Pope D, Pourmalek F, Qato D, Quistberg DA, Rafay A, Rahimi K, Rahimi-Movaghar V, ur Rahman S, Raju M, Rana SM, Refaat A, Ronfani L, Roy N, Pimienta TG, Sahraian MA, Salomon JA, Sampson U, Santos IS, Sawhney M, Sayinzoga F, Schneider IJ, Schumacher A, Schwebel DC, Seedat S, Sepanlou SG, Servan-Mori EE, Shakh-Nazarova M, Sheikhbahaei S, Shibuya K, Shin HH, Shiue I, Sigfusdottir ID, Silberberg DH, Silva AP, Singh JA, Skirbekk V, Sliwa K, Soshnikov SS, Sposato LA, Sreeramareddy CT, Stroumpoulis K, Sturua L, Sykes BL, Tabb KM, Talongwa RT, Tan F, Teixeira CM, Tenkorang EY, Terkawi AS, Thorne-Lyman AL, Tirschwell DL, Towbin JA, Tran BX, Tsilimbaris M, Uchendu US, Ukwaja KN, Undurraga EA, Uzun SB, Vallely AJ, van Gool CH, Vasankari TJ, Vavilala MS, Venketasubramanian N, Villalpando S, Violante FS, Vlassov VV, Vos T, Waller S, Wang H, Wang L, Wang X, Wang Y, Weichenthal S, Weiderpass E, Weintraub RG, Westerman R, Wilkinson JD, Woldeyohannes SM, Wong JQ, Wordofa MA, Xu G, Yang YC, Yano Y, Yentur GK, Yip P, Yonemoto N, Yoon SJ, Younis MZ, Yu C, Jin KY, El Sayed Zaki M, Zhao Y, Zheng Y, Zhou M, Zhu J, Zou XN, Lopez AD, Naghavi M, Murray CJ, Lozano R. Global, regional, and national levels and causes of maternal mortality during 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2014;384:980–1004. - PMC - PubMed
-
- Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3) JAMA. 2016;315:801–810. - PMC - PubMed
-
- Rhodes A, Evans LE, Alhazzani W, Levy MM, Antonelli M, Ferrer R, Kumar A, Sevransky JE, Sprung CL, Nunnally ME, Rochwerg B, Rubenfeld GD, Angus DC, Annane D, Beale RJ, Bellinghan GJ, Bernard GR, Chiche JD, Coopersmith C, De Backer DP, French CJ, Fujishima S, Gerlach H, Hidalgo JL, Hollenberg SM, Jones AE, Karnad DR, Kleinpell RM, Koh Y, Lisboa TC, Machado FR, Marini JJ, Marshall JC, Mazuski JE, McIntyre LA, McLean AS, Mehta S, Moreno RP, Myburgh J, Navalesi P, Nishida O, Osborn TM, Perner A, Plunkett CM, Ranieri M, Schorr CA, Seckel MA, Seymour CW, Shieh L, Shukri KA, Simpson SQ, Singer M, Thompson BT, Townsend SR, Van der Poll T, Vincent JL, Wiersinga WJ, Zimmerman JL, Dellinger RP. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016. Intensive Care Med. 2017;43:304–377. - PubMed
-
- World Health Organization. Statement on maternal sepsis. [cited 10 January 2021]. Available from: https://apps.who.int/iris/handle/10665/2546082017 .
-
- Khan KS, Wojdyla D, Say L, Gülmezoglu AM, Van Look PF. WHO analysis of causes of maternal death: a systematic review. Lancet. 2006;367:1066–1074. - PubMed
LinkOut - more resources
Full Text Sources