Tear Levels of Inflammatory Cytokines in Keratoconus: A Meta-Analysis of Case-Control and Cross-Sectional Studies
- PMID: 34631885
- PMCID: PMC8497143
- DOI: 10.1155/2021/6628923
Tear Levels of Inflammatory Cytokines in Keratoconus: A Meta-Analysis of Case-Control and Cross-Sectional Studies
Abstract
Purpose: To assess the tear levels of inflammatory cytokines in patients with keratoconus (KC).
Design: Systemic review and meta-analysis.
Methods: The following electronic databases and search engine were searched: PubMed, EMBASE, Web of Science, and Google Scholar. A systematic search of all relevant studies published through January 2021 was conducted, and the standardized mean difference (SMD) and 95% confidence interval (CI) of cytokine levels were calculated to estimate the pooled effects. Sensitivity analysis, subgroup analysis, and metaregression were applied to explore the sources of heterogeneity.
Results: A total of 7 studies with 374 participants (374 eyes) from clinical studies were included. The tear levels of interleukin-1 beta (IL-1β), interleukin-6 (IL-6), and tumor necrosis factor alpha (TNF-α) were significantly increased in KC compared with normal controls. The SMD of IL-1β was 1.93 (95% CI 0.22 to 3.65, P = 0.03). The SMD of IL-6 was 1.22 (95% CI 0.59 to 1.84, P < 0.001). The SMD of TNF-α was 1.75 (95% CI 0.66 to 2.83, P = 0.002). There was no significant difference between the two groups on interleukin-4 (IL-4) and interleukin-10 (IL-10). The SMD for IL-4 was 2.36 (95% CI -0.28 to 5.00, P = 0.08) and for IL-10 was 0.30 (95% CI -1.29 to 1.89, P = 0.71). Meta-regression analysis indicated that the heterogeneity maybe significantly correlated with the method of detection, the different ages, and the source of population.
Conclusions: Our meta-analysis demonstrated that proinflammatory cytokines IL-1β, IL-6, and TNF-α were increased, indicating that cytokine profile changed in KC tears and inflammation may play an important role in the pathogenesis and development of KC.
Copyright © 2021 Huan Zhang et al.
Conflict of interest statement
The authors declare that they have no conflicts of interest.
Figures
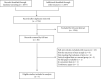





References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

