Probable Change of Sleep Parameters after Resection and Reconstruction Surgeries in Patients with Oral Cavity or Oropharyngeal Cancers
- PMID: 34631887
- PMCID: PMC8500743
- DOI: 10.1155/2021/7408497
Probable Change of Sleep Parameters after Resection and Reconstruction Surgeries in Patients with Oral Cavity or Oropharyngeal Cancers
Abstract
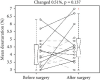
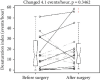
In patients of oral cavity or oropharyngeal cancers, resection of the tumor and reconstruction of the defect may reduce the framework, add a bulky flap, alter the tissue flexibility, and contribute to postoperative obstructive sleep apnea (OSA). Postoperative OSA and the potential consequences may decrease the survival rate and reduce patients' quality of life. It is unclear whether the surgery is associated with postoperative OSA. Here, we compared the polysomnographies (PSGs) before and after the surgery in 15 patients of oral cavity or oropharyngeal cancers (out of 68 patients of head and neck cancers) without a chemo- or radio-therapy. Each patient received the second PSG before the start of any indicated adjuvant therapy to prevent its interference. There were 14 men and 1 woman, with a mean age and a standard deviation (SD, same in the following) of 56.2 ± 12.8 years. There were 6 tongue cancers, 5 buccal cancers, 2 tonsil cancer, 1 lower gum cancer, and 1 trigone cancer. The results show that the surgery changed sleep parameters insignificantly in apnea-hypopnea index (AHI), mean oxyhemoglobin saturation of pulse oximetry (SpO2), minimum SpO2, mean desaturation, and desaturation index but increased mean heart rate in the patients with free flaps. These results hint that the effect of surgery on developing OSA was small in this sample, with a longer plate or a larger framework for a bulkier free flap. It needs future studies with a large sample size to generalize this first observation.
Copyright © 2021 Ethan I. Huang et al.
Conflict of interest statement
The authors declare no competing interests.
Figures




References
-
- Trimarchi M., Rampi A., Vinciguerra A., Polizzi E., Policaro N. S., Gastaldi G. Palatal prosthetic rehabilitation in patients affected by cocaine-induced midline destructive lesions. Journal of Biological Regulators and Homeostatic Agents . 2020;34(6 Suppl. 3):59–68. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

