Lymphocutaneous Sporotrichosis Refractory to First-Line Treatment
- PMID: 34659843
- PMCID: PMC8514908
- DOI: 10.1155/2021/9453701
Lymphocutaneous Sporotrichosis Refractory to First-Line Treatment
Abstract
Sporotrichosis is a fungal infection endemic in Latin America and has been attributed to the thermodimorphic fungus of the genus Sporothrix. Transmission to humans occurs during a traumatic injury with soil or organic material; additionally, lesions caused by infected cats play an important role in the epidemiology of the disease. The classic treatment of sporotrichosis is performed with itraconazole or potassium iodide; second-line medications, such as amphotericin B and terbinafine, can alternatively be used in cases of first-line drug failure. In the present study, a patient with lymphocutaneous sporotrichosis in the right upper limb exhibited intolerance to itraconazole and potassium iodide, additionally during the period of use; these drugs did not control skin lesions. In this patient, amphotericin B deoxycholate and its liposomal version were used in this patient; and complete recovery of the lesions was observed.
Copyright © 2021 Walter Belda Jr. et al.
Conflict of interest statement
The authors declare that there are no conflicts of interest regarding the publication of this article.
Figures


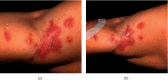

References
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

