Efficacy and safety of propranolol in infants with heart failure due to moderate-to-large ventricular septal defect (VSD-PHF study) - A prospective randomized trial
- PMID: 34667404
- PMCID: PMC8457270
- DOI: 10.4103/apc.APC_94_21
Efficacy and safety of propranolol in infants with heart failure due to moderate-to-large ventricular septal defect (VSD-PHF study) - A prospective randomized trial
Abstract
Aims: The utility of beta-blocker therapy in infants with heart failure (HF) due to significant left-to-right shunt lesions is not known. The study aimed to assess the efficacy and safety of propranolol in infants with HF due to moderate-to-large ventricular septal defect (VSD).
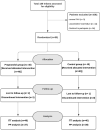
Methods: The prospective randomized trial included 80 infants with HF and moderate-to-large VSD, randomly allocated to receive either conventional therapy alone (n = 40) or propranolol plus conventional therapy (n = 40). The primary endpoint was a composite of all-cause mortality, hospitalization for HF and/or chest infection, and referral for surgery. The secondary clinical outcomes were the individual components of the composite endpoint. In addition, the patients were followed up to detect safety outcomes, for example, bronchospasm, bradyarrhythmia, and worsening HF symptoms.
Results: The addition of propranolol therapy to the conventional medications did not result in significant improvement in the primary composite endpoint (32.50% vs. 52.50%; P = 0.07). There was a trend toward improvement, but the study is underpowered for this important question. However, propranolol therapy significantly decreased the risk of hospitalization (12.50% vs. 32.50%; P = 0.03) and worsening of Ross HF class (5.41% vs. 28.21%; P = 0.01) as compared to conventional therapy (estimated number needed to treat = 5). Propranolol did not result in any significant safety concerns in these infants except bronchospasm in an infant.
Conclusions: Propranolol therapy in infants with significant left-to-right shunt may prevent worsening in HF symptoms and hospitalization and is well tolerated. However, it does not reduce mortality or need for surgery.
Keywords: Beta-blocker; left-to-right shunt; pediatric heart failure; propranolol; ventricular septal defect.
Copyright: © 2021 Annals of Pediatric Cardiology.
Conflict of interest statement
There are no conflicts of interest.
Figures
Similar articles
-
Biventricular pacing (cardiac resynchronization therapy): an evidence-based analysis.Ont Health Technol Assess Ser. 2005;5(13):1-60. Epub 2005 Sep 1. Ont Health Technol Assess Ser. 2005. PMID: 23074464 Free PMC article.
-
Propranolol treatment of congestive heart failure in infants with congenital heart disease: The CHF-PRO-INFANT Trial. Congestive heart failure in infants treated with propanol.Int J Cardiol. 2001 Jul;79(2-3):167-73. doi: 10.1016/s0167-5273(01)00413-2. Int J Cardiol. 2001. PMID: 11461738 Clinical Trial.
-
The Effectiveness of Eplerenone vs Spironolactone on Left Ventricular Systolic Function, Hospitalization and Cardiovascular Death in Patients With Chronic Heart Failure-HFrEF.Med Arch. 2023 Apr;77(2):105-111. doi: 10.5455/medarh.2023.77.105-111. Med Arch. 2023. PMID: 37260796 Free PMC article. Clinical Trial.
-
Efficacy and safety of carvedilol in treatment of heart failure with chronic kidney disease: a meta-analysis of randomized trials.Circ Heart Fail. 2011 Jan;4(1):18-26. doi: 10.1161/CIRCHEARTFAILURE.109.932558. Epub 2010 Oct 29. Circ Heart Fail. 2011. PMID: 21036889 Clinical Trial.
-
Implantable cardioverter defibrillators. Prophylactic use: an evidence-based analysis.Ont Health Technol Assess Ser. 2005;5(14):1-74. Epub 2005 Sep 1. Ont Health Technol Assess Ser. 2005. PMID: 23074465 Free PMC article.
Cited by
-
Cardiomyocyte proliferation and regeneration in congenital heart disease.Pediatr Discov. 2024 Sep;2(3):e2501. doi: 10.1002/pdi3.2501. Epub 2024 Aug 12. Pediatr Discov. 2024. PMID: 39308981 Free PMC article.
-
Pediatric cardiology: Is India self-reliant?Ann Pediatr Cardiol. 2021 Jul-Sep;14(3):253-259. doi: 10.4103/apc.apc_153_21. Epub 2021 Aug 13. Ann Pediatr Cardiol. 2021. PMID: 34667394 Free PMC article. No abstract available.
-
Beta-blocker therapy in pediatric heart failure: 50 years lost to improve pharmacotherapy of a deadly disease.Ann Pediatr Cardiol. 2021 Jul-Sep;14(3):341-342. doi: 10.4103/apc.apc_126_21. Epub 2021 Aug 26. Ann Pediatr Cardiol. 2021. PMID: 34667405 Free PMC article. No abstract available.
-
Congenital Heart Disease: The State-of-the-Art on Its Pharmacological Therapeutics.J Cardiovasc Dev Dis. 2022 Jun 26;9(7):201. doi: 10.3390/jcdd9070201. J Cardiovasc Dev Dis. 2022. PMID: 35877563 Free PMC article. Review.
-
Pediatric cardiology: In search for evidence.Ann Pediatr Cardiol. 2023 Sep-Oct;16(5):311-315. doi: 10.4103/apc.apc_47_24. Epub 2024 Apr 1. Ann Pediatr Cardiol. 2023. PMID: 38766456 Free PMC article. No abstract available.
References
-
- Moe DG, Guntheroth WG. Spontaneous closure of uncomplicated ventricular septal defect. Am J Cardiol. 1987;60:674–8. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous