Modified Hidden Blood Loss Based on Drainage in Posterior Surgery on Lumbar Stenosis Syndrome with Rheumatoid Arthritis
- PMID: 34672095
- PMCID: PMC8654656
- DOI: 10.1111/os.13157
Modified Hidden Blood Loss Based on Drainage in Posterior Surgery on Lumbar Stenosis Syndrome with Rheumatoid Arthritis
Abstract
Objective: Publications on hidden blood loss (HBL) after posterior lumbar interbody fusion (PLIF) for lumbar spine stenosis syndrome (LSS) have been reported, but the modified HBL (mHBL) was different from HBL obtained by classical formula and there are few studies on lumbar spine hemorrhage with rheumatoid arthritis (RA). Therefore, the aim of our study is to respectively evaluate the importance of hidden blood loss (HBL) and modified HBL (mHBL) after posterior lumbar interbody fusion (PLIF) in patients diagnosed with LSS and RA, to explore the correlation between RA activity and HBL as well as mHBL.
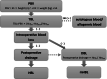
Methods: A total of 61 patients (nine males and 52 females) diagnosed with LSS and RA who underwent PLIF were included. Data contained demographics, RA-related parameters such as duration of RA, Steinbrocker classification (used to evaluated RA activity), the disease-modifying anti-rheumatic drugs (DMARDs), osteoporosis and total knee arthroplasty; operation and hemorrhage parameters. Then HBL and mHBL were calculated by Gross formula and modified formula, respectively. Subgroup analysis on HBL and mHBL was performed based on gender, age (≤60 years and ˃60 years), different number of surgical segments (single segment, double segment, and ≥3 segments), and taking DMARDs or not. ANOVA analysis was performed on HBL and mHBL in different surgery segment number and Steinbrocker classification of RA. Independent sample t-test was used in comparison of gender and age, as well as in comparison between HBL and mHBL based on whether the patient took DMARDs or not. Furthermore, paired t-test was used to compare the volume between HBL and mHBL.
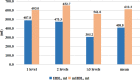
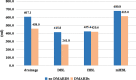
Results: The mean age and duration of RA was 65.2 ± 9.3 years and 14.3 ± 10.7 years, respectively. There were 13 grade I cases, 34 grade II cases, and 14 grade III cases as assessed by Steinbrocker classification and the most common anti-RA drugs were DMARDs (57.4%). The mean intraoperative bleeding, drainage, and blood loss in drainage (DBL) was 453.3 ± 377.8 mL, 489.1 ± 253.8 mL, and 304.6 ± 156.3 mL, respectively. There was no difference on HBL and mHBL in gender. HBL and mHBL was larger in patients over 60 years (P = 0.040 and P = 0.023). There were differences in intraoperative blood loss, drainage, and DBL based on different number of segments but not in HBL and mHBL, or on Steinbrocker classification. DBL was lower in DMARDs group than non-drugged group (P = 0.03), while HBL and mHBL were both of no significance. The comparison of HBL and mHBL showed statistical difference (P < 0.001), suggesting that mHBL volume is larger than HBL.
Conclusions: Patients diagnosed as LSS with RA have amounts of HBL or mHBL after PLIF. HBL or mHBL is not associated with RA activity, which may not increase in RA patients compared with common ones. Taking DMARDs may reduce postoperative DBL. The fact that mHBL is larger than HBL provides an all-round basis for measuring factual HBL.
Keywords: Hidden blood loss; Lumbar stenosis syndrome; Modified hidden blood loss; Posterior lumbar interbody fusion; Rheumatoid arthritis.
© 2021 The Authors. Orthopaedic Surgery published by Chinese Orthopaedic Association and John Wiley & Sons Australia, Ltd.
Figures
Similar articles
-
Blood Loss of Posterior Lumbar Interbody Fusion on Lumbar Stenosis in Patients With Rheumatoid Arthritis: A Case-Control Study.Spine (Phila Pa 1976). 2019 Sep 1;44(17):E1045-E1052. doi: 10.1097/BRS.0000000000003037. Spine (Phila Pa 1976). 2019. PMID: 30985568
-
[Analysis of perioperative blood loss of posterior lumbar interbody fusion on lumbar spondylolisthesis in patients with rheumatoid arthritis].Zhonghua Yi Xue Za Zhi. 2021 Mar 23;101(11):792-797. doi: 10.3760/cma.j.cn112137-20201009-02791. Zhonghua Yi Xue Za Zhi. 2021. PMID: 33765720 Chinese.
-
The further exploration of hidden blood loss in posterior lumbar fusion surgery.Orthop Traumatol Surg Res. 2017 Jun;103(4):527-530. doi: 10.1016/j.otsr.2017.01.011. Epub 2017 Mar 11. Orthop Traumatol Surg Res. 2017. PMID: 28300704
-
Complete persistent remission of rheumatoid arthritis after COVID-19 infection - A rare case and literature review.Monaldi Arch Chest Dis. 2022 Jun 8;93(1). doi: 10.4081/monaldi.2022.2195. Monaldi Arch Chest Dis. 2022. PMID: 35678534 Review.
-
Effect of Rheumatoid Arthritis on Postoperative Outcomes in Patients with Lumbar Spinal Disorders: A Systematic Review and Meta-Analysis.Global Spine J. 2025 Jun;15(5):2789-2797. doi: 10.1177/21925682251318265. Epub 2025 Jan 29. Global Spine J. 2025. PMID: 39881528 Free PMC article. Review.
Cited by
-
Risk Factors of Total Blood Loss and Hidden Blood Loss in Patients with Adolescent Idiopathic Scoliosis: A Retrospective Study.Biomed Res Int. 2022 May 27;2022:9305190. doi: 10.1155/2022/9305190. eCollection 2022. Biomed Res Int. 2022. PMID: 35669721 Free PMC article.
-
Utility of postoperative laboratory testing after posterior spinal fusion for adolescent idiopathic scoliosis.Spine Deform. 2024 Mar;12(2):375-381. doi: 10.1007/s43390-023-00771-1. Epub 2023 Oct 26. Spine Deform. 2024. PMID: 37884756
References
-
- Brecher ME, Monk T, Goodnough LT. A standardized method for calculating blood loss. Transfusion, 1997, 37: 1070–1074. - PubMed
-
- Ogura Y, Dimar IJ, Gum JL, et al. Hidden blood loss following 2‐ to 3‐level posterior lumbar fusion. Spine J, 2019, 19: 2003–2006. - PubMed
-
- Sehat KR, Evans RL, Newman JH. Hidden blood loss following hip and knee arthroplasty. Correct management of blood loss should take hidden loss into account. J Bone Joint Surg Br, 2004, 86: 561–565. - PubMed
-
- Korovessis P. Hidden blood loss in spine surgery for A1‐A3 thoracolumbar fractures. Comparison between three approaches. J Invest Surg, 2019, 32: 761–762. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

