A problem-based approach in musculoskeletal ultrasonography: heel pain in adults
- PMID: 34674456
- PMCID: PMC8696136
- DOI: 10.14366/usg.21069
A problem-based approach in musculoskeletal ultrasonography: heel pain in adults
Abstract
Musculoskeletal ultrasonography (US) has unique advantages, such as excellent spatial resolution for superficial structures, the capability for dynamic imaging, and the ability for direct correlation and provocation of symptoms. For these reasons, US is increasingly used to evaluate problems in small joints, such as the foot and ankle. However, it is almost impossible to evaluate every anatomic structure within a limited time. Therefore, US examinations can be faster and more efficient if radiologists know where to look and image patients with typical symptoms. In this review, common etiologies of heel pain are discussed in a problem-based manner. Knowing the common pain sources and being familiar with their US findings will help radiologists to perform accurate and effective US examinations.
Keywords: Ankle; Foot; Heel; Pain; Ultrasonography; Ultrasound.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures
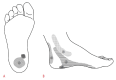
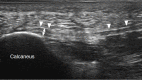
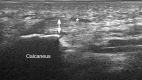

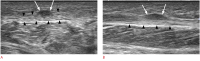
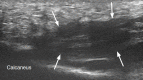
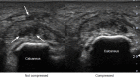

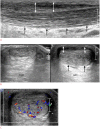
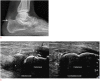



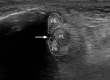
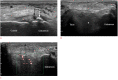
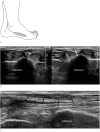
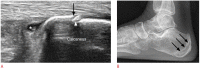
References
-
- Tu P. Heel pain: diagnosis and management. Am Fam Physician. 2018;97:86–93. - PubMed
-
- Thomas JL, Christensen JC, Kravitz SR, Mendicino RW, Schuberth JM, Vanore JV, et al. The diagnosis and treatment of heel pain: a clinical practice guideline-revision 2010. J Foot Ankle Surg. 2010;49(3 Suppl):S1–S19. - PubMed
-
- Lareau CR, Sawyer GA, Wang JH, DiGiovanni CW. Plantar and medial heel pain: diagnosis and management. J Am Acad Orthop Surg. 2014;22:372–380. - PubMed
-
- Rio E, Mayes S, Cook J. Heel pain: a practical approach. Aust Fam Physician. 2015;44:96–101. - PubMed
-
- Gibbon WW, Long G. Ultrasound of the plantar aponeurosis (fascia) Skeletal Radiol. 1999;28:21–26. - PubMed
LinkOut - more resources
Full Text Sources

