Evaluation of the Factors Affecting the Cure Rate of Cervical Intra-Epithelial Neoplasia Recurrence Using Defective Models
- PMID: 34698658
- PMCID: PMC8957688
- DOI: 10.34172/jrhs.2021.56
Evaluation of the Factors Affecting the Cure Rate of Cervical Intra-Epithelial Neoplasia Recurrence Using Defective Models
Abstract
Background: Treatment of cervical intraepithelial neoplasia is very important since if it remains untreated, it may progress to cervical cancer. It is usually treated with excisional surgery. This study aimed to find the factors affecting the cure rate of cervical intraepithelial neoplasia recurrence after surgery using defective models.
Study design: A retrospective cohort study.
Methods: Excisional surgery was performed on 307 patients with high-grade cervical intraepithelial neoplasia, from 2009 to 2017. The patients were followed up until recurrence based on histopathology report. Hematologic factors were measured before surgery. The cure rates were estimated using defective models with a Gamma frailty term and the results were compared.
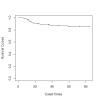
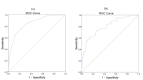
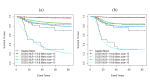
Results: Neutrophil-to-lymphocyte ratio (NLR) (P<0.001) and excised mass size (P<0.001) had significant impacts on cure rates, and their cut-off values were 1.9 (P<0.001) and 15 mm2 (P<0.001), respectively. Patients with lower neutrophil-to-lymphocyte ratios and larger excised tissues had higher cure rates. Defective 3-parameter Gompertz distribution with gamma frailty term had the best fit to the data, and its estimated cure rates were 98% among patients with an excised mass size of > 15 mm2 and NLR of <1.9, 84% among patients with an excised mass size of >15 mm2 and NLR of >1.9, 79% among patients with an excised mass size of <15 mm2 and NLR of <1.9, and 30% among patients with an excised mass size of <15 mm2 and NLR of >1.9.
Conclusion: Cervical intraepithelial neoplasia must be identified and treated before its progress. Excision of more tissues during excisional surgery, especially when the NLR of the patient is high, can help to prevent cervical intraepithelial neoplasia recurrence.
Keywords: Cervical intra-epithelial neoplasia; Cure rate; Defective models; Survival analysis.
References
-
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394–424. - PubMed
-
- Garcia F, Hatch KD, Berek JS. Intraepithelial Disease of the Cervix, Vagina, and Vulva. 15th ed. Berek and Novak’s Gynecology. Berek JS, editor, Philadelphia: Lippincott Williams and Wilkins 2012; p: 574-618.
-
- IARC. IARC handbooks of cancer prevention: cervix cancer screening. Vol 10. IARC Press. 2005.