Imaging diagnosis of autoimmune pancreatitis: computed tomography and magnetic resonance imaging
- PMID: 34698963
- PMCID: PMC8578112
- DOI: 10.1007/s10396-021-01145-8
Imaging diagnosis of autoimmune pancreatitis: computed tomography and magnetic resonance imaging
Abstract
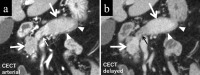
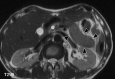
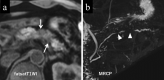
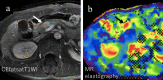
Autoimmune pancreatitis (AIP) is a pancreatic phenotype of IgG4-related systemic disease. Since its first description in the literature, characteristic imaging features have gradually become known to many clinicians encompassing various specialties in the past quarter century. CT and MRI have been the workhorses for imaging diagnosis of AIP. Typical features include sausage-like swelling of the focal or entire pancreas, duct-penetrating sign, a capsule-like rim of the affected lesions, and homogeneous delayed enhancement or enhanced duct sign after contrast administration, as well as characteristic combined findings reflecting coexisting pathologies in the other organs as a systemic disease. In this review, recent and future developments in CT and MRI that may help diagnose AIP are discussed, including restricted diffusion and perfusion and increased elasticity measured using MR.
Keywords: Autoimmune pancreatitis; Computed tomography; Diffusion-weighted image; IgG4; MR elastography.
© 2021. The Author(s).
Conflict of interest statement
The second author, Yasuo Takehara, is an endowed chair of a department financially supported by a private company; however, the status is irrelevant to the contents of this paper. Other authors declare that there are no conflicts of interest related to the contents of the article.
Figures




References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

