Modulation of immune-inflammatory responses through surface modifications of biomaterials to promote bone healing and regeneration
- PMID: 34721831
- PMCID: PMC8554547
- DOI: 10.1177/20417314211041428
Modulation of immune-inflammatory responses through surface modifications of biomaterials to promote bone healing and regeneration
Abstract
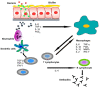
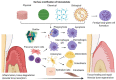
Control of inflammation is indispensable for optimal oral wound healing and tissue regeneration. Several biomaterials have been used to enhance the regenerative outcomes; however, the biomaterial implantation can ensure an immune-inflammatory response. The interface between the cells and the biomaterial surface plays a critical role in determining the success of soft and hard tissue regeneration. The initial inflammatory response upon biomaterial implantation helps in tissue repair and regeneration, however, persistant inflammation impairs the wound healing response. The cells interact with the biomaterials through extracellular matrix proteins leading to protein adsorption followed by recruitment, attachment, migration, and proliferation of several immune-inflammatory cells. Physical nanotopography of biomaterials, such as surface proteins, roughness, and porosity, is crucial for driving cellular attachment and migration. Similarly, modification of scaffold surface chemistry by adapting hydrophilicity, surface charge, surface coatings, can down-regulate the initiation of pro-inflammatory cascades. Besides, functionalization of scaffold surfaces with active biological molecules can down-regulate pro-inflammatory and pro-resorptive mediators' release as well as actively up-regulate anti-inflammatory markers. This review encompasses various strategies for the optimization of physical, chemical, and biological properties of biomaterial and the underlying mechanisms to modulate the immune-inflammatory response, thereby, promoting the tissue integration and subsequent soft and hard tissue regeneration potential of the administered biomaterial.
Keywords: Topography; implants; inflammation; oral disease; periodontitis; regeneration; scaffold.
© The Author(s) 2021.
Conflict of interest statement
Declaration of conflicting interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures


References
-
- Vishwakarma A, Bhise NS, Evangelista MB, et al.. Engineering immunomodulatory biomaterials to tune the inflammatory response. Trends Biotechnol 2016; 34: 470–482. - PubMed
-
- Kämmerling L, Fisher LE, Antmen E, et al.. Mitigating the foreign body response through ‘immune-instructive’ biomaterials. J Immunol Reg Med 2021; 12: 100040.
-
- Sculean A, Nikolidakis D, Nikou G, et al.. Biomaterials for promoting periodontal regeneration in human intrabony defects: a systematic review. Periodontol 2000 2015; 68: 182–216. - PubMed
-
- Vasconcelos DP, Águas AP, Barbosa MA, et al.. The inflammasome in host response to biomaterials: bridging inflammation and tissue regeneration. Acta Biomater 2019; 83: 1–12. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

