A Clinical Review of the Psychiatric Sequelae of Primary Hyperparathyroidism
- PMID: 34722014
- PMCID: PMC8549683
- DOI: 10.7759/cureus.19078
A Clinical Review of the Psychiatric Sequelae of Primary Hyperparathyroidism
Abstract
Despite one-quarter of patients with primary hyperparathyroidism (PHPT) experiencing psychiatric symptoms, there remains a dearth of literature regarding the diagnosis and further management of psychiatric sequelae in PHPT. We aim to review the literature pertaining to the epidemiology, disease presentation, pathophysiology, diagnostics, and therapeutics regarding psychiatric sequelae of PHPT with an emphasis on clinical pearls for practicing psychiatrists. A literature search was conducted using the US National Library of Medicine's PubMed resource using the following keywords in various combinations: primary hyperparathyroidism, neuropsychiatric, calcium, psychosis, mania, depression, catatonia, delirium, parathyroidectomy, and psychotropic medication. We discuss in depth all aspects of the diagnosis and management of psychiatric sequela in PHPT. We have also identified epidemiological trends, discussed the most common clinical presentations, and postulated possible mechanisms for psychiatric symptoms in PHPT. Psychiatrists should maintain diagnostic suspicion for PHPT in older adult female patients presenting with new-onset psychiatric illness. Several mechanisms involving the following may explain the variety of psychiatric symptoms in PHPT: tyrosine hydroxylase, parathyroid hormone, interleukin-6, monoamine oxidase, calcium, and the sodium-potassium adenosine triphosphatase transporter. We recommend psychiatrists take a symptom-oriented approach to management. Treating a patient's psychosis, mania, depression, catatonia, delirium, or eating disorder pathology via conventional therapeutics seems like a rational approach despite the underlying medical etiology. Only parathyroidectomy has been proven to be definitive in the complete amelioration of psychiatric symptoms.
Keywords: adult primary hyperparathyroidism; behavioral endocrinology; clinical neuroscience; consultation liaison psychiatry; psychosomatic psychiatry.
Copyright © 2021, Serdenes et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
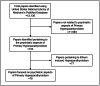
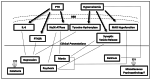
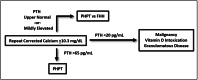
Similar articles
-
Mild primary hyperparathyroidism: a literature review.Oncologist. 2014 Sep;19(9):919-29. doi: 10.1634/theoncologist.2014-0084. Epub 2014 Jul 25. Oncologist. 2014. PMID: 25063228 Free PMC article. Review.
-
Relation of hyperparathyroidism and hypercalcemia to bipolar and psychotic disorders.Proc (Bayl Univ Med Cent). 2022 Apr 8;35(4):540-542. doi: 10.1080/08998280.2022.2057211. eCollection 2022. Proc (Bayl Univ Med Cent). 2022. PMID: 35754598 Free PMC article.
-
Primary hyperparathyroidism.Nat Rev Endocrinol. 2018 Feb;14(2):115-125. doi: 10.1038/nrendo.2017.104. Epub 2017 Sep 8. Nat Rev Endocrinol. 2018. PMID: 28885621 Free PMC article. Review.
-
Parathyroidectomy for primary hyperparathyroidism in octogenarians and nonagenarians: a plea for early surgical referral.Arch Surg. 2003 Aug;138(8):867-71. doi: 10.1001/archsurg.138.8.867. Arch Surg. 2003. PMID: 12912745
-
Primary hyperparathyroidism: Update on presentation, diagnosis, and management in primary care.Can Fam Physician. 2011 Feb;57(2):184-9. Can Fam Physician. 2011. PMID: 21321169 Free PMC article.
Cited by
-
Risk of neuropsychiatric disorders in primary hyperparathyroidism: Parathyroidectomy versus nonoperative management.World J Surg. 2025 Jan;49(1):106-114. doi: 10.1002/wjs.12285. Epub 2024 Jul 14. World J Surg. 2025. PMID: 39004613
-
An Analysis of Primary Hyperparathyroidism in Association with Depression or Anxiety.Diseases. 2025 Feb 12;13(2):54. doi: 10.3390/diseases13020054. Diseases. 2025. PMID: 39997061 Free PMC article. Review.
-
A Case of Gitelman Syndrome with Hypercalcemia Secondary to Primary Hyperparathyroidism.Case Rep Endocrinol. 2022 Jun 25;2022:1098222. doi: 10.1155/2022/1098222. eCollection 2022. Case Rep Endocrinol. 2022. PMID: 35795477 Free PMC article.
-
Analysis of Clinical and Biochemical Parameters and the Effectiveness of Surgical Treatment in Patients with Primary Hyperparathyroidism: A Single-Center Study.J Clin Med. 2025 Feb 4;14(3):996. doi: 10.3390/jcm14030996. J Clin Med. 2025. PMID: 39941666 Free PMC article.
-
Primary Hyperparathyroidism Causing Psychosis: A Case Report.Cureus. 2022 Nov 27;14(11):e31935. doi: 10.7759/cureus.31935. eCollection 2022 Nov. Cureus. 2022. PMID: 36582554 Free PMC article.
References
-
- Hyperparathyroidism. Fraser WD. Lancet. 2009;374:145–158. - PubMed
-
- Epidemiology of primary hyperparathyroidism. Melton LJ III. J Bone Miner Res. 1991;6:0. - PubMed
-
- The prevalence of undiagnosed and unrecognized primary hyperparathyroidism: a population-based analysis from the electronic medical record. Press DM, Siperstein AE, Berber E, et al. Surgery. 2013;154:1232–1238. - PubMed
-
- Psychiatric morbidity in primary hyperparathyroidism. Joborn C, Hetta J, Johansson H, Rastad J, Agren H, Akerström G, Ljunghall S. World J Surg. 1988;12:476–480. - PubMed
-
- Hypercalcemia and "primary" hyperparathyroidism during lithium therapy. Shapiro HI, Davis KA. Am J Psychiatry. 2015;172:12–15. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
