The Incidence of Breast Cancer Recurrence 10-32 Years After Primary Diagnosis
- PMID: 34747484
- PMCID: PMC8902439
- DOI: 10.1093/jnci/djab202
The Incidence of Breast Cancer Recurrence 10-32 Years After Primary Diagnosis
Abstract
Background: Extended, more effective breast cancer treatments have increased the prevalence of long-term survivors. We investigated the risk of late breast cancer recurrence (BCR), 10 years or more after primary diagnosis, and associations between patient and tumor characteristics at primary diagnosis and late BCR up to 32 years after primary breast cancer diagnosis.
Methods: Using the Danish Breast Cancer Group clinical database, we identified all women with an incident early breast cancer diagnosed during 1987-2004. We restricted to women who survived 10 years without a recurrence or second cancer (10-year disease-free survivors) and followed them from 10 years after breast cancer diagnosis date until late recurrence, death, emigration, second cancer, or December 31, 2018. We calculated incidence rates per 1000 person-years and cumulative incidences for late BCR, stratifying by patient and tumor characteristics. Using Cox regression, we calculated adjusted hazard ratios for late BCR accounting for competing risks.
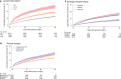
Results: Among 36 924 women with breast cancer, 20 315 became 10-year disease-free survivors. Of these, 2595 developed late BCR (incidence rate = 15.53 per 1000 person-years, 95% confidence interval = 14.94 to 16.14; cumulative incidence = 16.6%, 95% confidence interval = 15.8% to 17.5%) from year 10 to 32 after primary diagnosis. Tumor size larger than 20 mm, lymph node-positive disease, and estrogen receptor-positive tumors were associated with increased cumulative incidences and hazards for late BCR.
Conclusions: Recurrences continued to occur up to 32 years after primary diagnosis. Women with high lymph node burden, large tumor size, and estrogen receptor-positive tumors had increased risk of late recurrence. Such patients may warrant extended surveillance, more aggressive treatment, or new therapy approaches.
© The Author(s) 2021. Published by Oxford University Press.
Figures


Comment in
-
Prevention of Late Recurrence: An Increasingly Important Target for Breast Cancer Research and Control.J Natl Cancer Inst. 2022 Mar 8;114(3):340-341. doi: 10.1093/jnci/djab203. J Natl Cancer Inst. 2022. PMID: 34747495 Free PMC article. No abstract available.
References
-
- Peto R, Boreham J, Clarke M, Davies C, Beral V.. UK and USA breast cancer deaths down 25% in year 2000 at ages 20-69 years. Lancet Lond Engl. 2000;355(9217):1822. doi:10.1016/S0140-6736(00)02277-7. - PubMed
-
- Howell A, Cuzick J, Baum M, et al. Results of the ATAC (Arimidex, Tamoxifen, Alone or in Combination) trial after completion of 5 years’ adjuvant treatment for breast cancer. Lancet Lond Engl. 2005;365(9453):60–62. doi:10.1016/S0140-6736(04)17666-6. - PubMed
-
- Goss PE, Chambers AF.. Does tumour dormancy offer a therapeutic target? Nat Rev Cancer. 2010;10(12):871–877. doi:10.1038/nrc2933. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

