Deep learning identified pathological abnormalities predictive of graft loss in kidney transplant biopsies
- PMID: 34757124
- PMCID: PMC10285669
- DOI: 10.1016/j.kint.2021.09.028
Deep learning identified pathological abnormalities predictive of graft loss in kidney transplant biopsies
Abstract
Interstitial fibrosis, tubular atrophy, and inflammation are major contributors to kidney allograft failure. Here we sought an objective, quantitative pathological assessment of these lesions to improve predictive utility and constructed a deep-learning-based pipeline recognizing normal vs. abnormal kidney tissue compartments and mononuclear leukocyte infiltrates. Periodic acid- Schiff stained slides of transplant biopsies (60 training and 33 testing) were used to quantify pathological lesions specific for interstitium, tubules and mononuclear leukocyte infiltration. The pipeline was applied to the whole slide images from 789 transplant biopsies (478 baseline [pre-implantation] and 311 post-transplant 12-month protocol biopsies) in two independent cohorts (GoCAR: 404 patients, AUSCAD: 212 patients) of transplant recipients to correlate composite lesion features with graft loss. Our model accurately recognized kidney tissue compartments and mononuclear leukocytes. The digital features significantly correlated with revised Banff 2007 scores but were more sensitive to subtle pathological changes below the thresholds in the Banff scores. The Interstitial and Tubular Abnormality Score (ITAS) in baseline samples was highly predictive of one-year graft loss, while a Composite Damage Score in 12-month post-transplant protocol biopsies predicted later graft loss. ITASs and Composite Damage Scores outperformed Banff scores or clinical predictors with superior graft loss prediction accuracy. High/intermediate risk groups stratified by ITASs or Composite Damage Scores also demonstrated significantly higher incidence of estimated glomerular filtration rate decline and subsequent graft damage. Thus, our deep-learning approach accurately detected and quantified pathological lesions from baseline or post-transplant biopsies and demonstrated superior ability for prediction of post-transplant graft loss with potential application as a prevention, risk stratification or monitoring tool.
Keywords: deep learning; graft survival; kidney transplantation; renal pathology.
Copyright © 2021 International Society of Nephrology. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
All the other authors declared no competing interests.
Figures
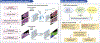



Similar articles
-
A large-scale retrospective study enabled deep-learning based pathological assessment of frozen procurement kidney biopsies to predict graft loss and guide organ utilization.Kidney Int. 2024 Feb;105(2):281-292. doi: 10.1016/j.kint.2023.09.031. Epub 2023 Nov 3. Kidney Int. 2024. PMID: 37923131 Free PMC article.
-
Utility of Serial Protocol Biopsies Performed After 1 Year in Predicting Long-Term Kidney Allograft Function According to Histologic Phenotype.Exp Clin Transplant. 2018 Aug;16(4):391-400. doi: 10.6002/ect.2016.0323. Epub 2017 Dec 5. Exp Clin Transplant. 2018. PMID: 29206090
-
Predictors of renal transplant histology at three months.Transplantation. 1999 May 15;67(9):1222-30. doi: 10.1097/00007890-199905150-00005. Transplantation. 1999. PMID: 10342313
-
Protocol biopsies in renal transplantation: prognostic value of structural monitoring.Kidney Int. 2007 Sep;72(6):690-7. doi: 10.1038/sj.ki.5002396. Epub 2007 Jun 27. Kidney Int. 2007. PMID: 17597702 Review.
-
Risk factors associated with the deterioration of renal function: the role of protocol biopsies.Prilozi. 2007 Jul;28(1):291-302. Prilozi. 2007. PMID: 17932475 Review.
Cited by
-
Towards accurate and efficient diagnoses in nephropathology: An AI-based approach for assessing kidney transplant rejection.Comput Struct Biotechnol J. 2024 Aug 16;24:571-582. doi: 10.1016/j.csbj.2024.08.011. eCollection 2024 Dec. Comput Struct Biotechnol J. 2024. PMID: 39258238 Free PMC article.
-
Artificial intelligence-enhanced interpretation of kidney transplant biopsy: focus on rejection.Curr Opin Organ Transplant. 2025 Jun 1;30(3):201-207. doi: 10.1097/MOT.0000000000001213. Epub 2025 Apr 1. Curr Opin Organ Transplant. 2025. PMID: 40171636 Free PMC article. Review.
-
Evaluating tubulointerstitial compartments in renal biopsy specimens using a deep learning-based approach for classifying normal and abnormal tubules.PLoS One. 2022 Jul 11;17(7):e0271161. doi: 10.1371/journal.pone.0271161. eCollection 2022. PLoS One. 2022. PMID: 35816495 Free PMC article.
-
Artificial intelligence in renal pathology: Current status and future.Biomol Biomed. 2023 Mar 16;23(2):225-234. doi: 10.17305/bjbms.2022.8318. Biomol Biomed. 2023. PMID: 36378066 Free PMC article. Review.
-
The Banff 2022 Kidney Meeting Work Plan: Data-driven refinement of the Banff Classification for renal allografts.Am J Transplant. 2024 Mar;24(3):350-361. doi: 10.1016/j.ajt.2023.10.031. Epub 2023 Nov 4. Am J Transplant. 2024. PMID: 37931753 Free PMC article.
References
-
- Hunsicker LG. A survival advantage for renal transplantation. N Engl J Med. 1999;341:1762–1763. - PubMed
-
- Furness PN, Taub N. Convergence of European Renal Transplant Pathology Assessment Procedures (CERTAP) Project. International variation in the interpretation of renal transplant biopsies: report of the CERTPAP project. Kidney Int. 2001;60:1998–2012. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

