Blood transfusion and the risk for infections in kidney transplant patients
- PMID: 34767576
- PMCID: PMC8589196
- DOI: 10.1371/journal.pone.0259270
Blood transfusion and the risk for infections in kidney transplant patients
Abstract
Background: Receipt of a red blood cell transfusion (RBCT) post-kidney transplantation may alter immunity which could predispose to subsequent infection.
Methods: We carried out a single-center, retrospective cohort study of 1,258 adult kidney transplant recipients from 2002 to 2018 (mean age 52, 64% male). The receipt of RBCT post-transplant (468 participants transfused, total 2,373 RBCT) was analyzed as a time-varying, cumulative exposure. Adjusted cox proportional hazards models were used to calculate hazard ratios (HR) for outcomes of bacterial or viral (BK or CMV) infection.
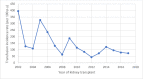
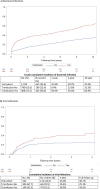
Results: Over a median follow-up of 3.8 years, bacterial infection occurred in 34% of participants at a median of 409 days post-transplant and viral infection occurred in 25% at a median of 154 days post-transplant. Transfusion was associated with a step-wise higher risk of bacterial infection (HR 1.35, 95%CI 0.95-1.91; HR 1.29, 95%CI 0.92-1.82; HR 2.63, 95%CI 1.94-3.56; HR 3.38, 95%CI 2.30-4.95, for 1, 2, 3-5 and >5 RBCT respectively), but not viral infection. These findings were consistent in multiple additional analyses, including accounting for reverse causality.
Conclusion: Blood transfusion after kidney transplant is associated with a higher risk for bacterial infection, emphasizing the need to use transfusions judiciously in this population already at risk for infections.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Clinical impact of early post-transplant red cell transfusions in kidney transplantation: a systematic review and meta-analysis.Front Transplant. 2023 Jul 10;2:1215130. doi: 10.3389/frtra.2023.1215130. eCollection 2023. Front Transplant. 2023. PMID: 38993906 Free PMC article. Review.
-
Transfused Red Blood Cell Characteristics and Kidney Transplant Outcomes Among Patients Receiving Early Posttransplant Transfusion.JAMA Netw Open. 2023 Sep 5;6(9):e2332821. doi: 10.1001/jamanetworkopen.2023.32821. JAMA Netw Open. 2023. PMID: 37707816 Free PMC article.
-
The association of venous thromboembolism with blood transfusion in kidney transplant patients.Transfusion. 2022 Dec;62(12):2480-2489. doi: 10.1111/trf.17154. Epub 2022 Nov 3. Transfusion. 2022. PMID: 36325656
-
Blood Transfusion and Adverse Graft-related Events in Kidney Transplant Patients.Kidney Int Rep. 2021 Feb 2;6(4):1041-1049. doi: 10.1016/j.ekir.2021.01.015. eCollection 2021 Apr. Kidney Int Rep. 2021. PMID: 33912754 Free PMC article.
-
Blood transfusion and infection after cardiac surgery.Ann Thorac Surg. 2013 Jun;95(6):2194-201. doi: 10.1016/j.athoracsur.2012.11.078. Epub 2013 May 3. Ann Thorac Surg. 2013. PMID: 23647857 Free PMC article. Review.
Cited by
-
Clinical impact of early post-transplant red cell transfusions in kidney transplantation: a systematic review and meta-analysis.Front Transplant. 2023 Jul 10;2:1215130. doi: 10.3389/frtra.2023.1215130. eCollection 2023. Front Transplant. 2023. PMID: 38993906 Free PMC article. Review.
-
Blood transfusions post kidney transplantation are associated with inferior allograft and patient survival-it is time for rigorous patient blood management.Front Nephrol. 2023 Jul 24;3:1236520. doi: 10.3389/fneph.2023.1236520. eCollection 2023. Front Nephrol. 2023. PMID: 37675353 Free PMC article.
-
Editorial: Future challenges and directions in determining allo-immunity in kidney transplantation.Front Immunol. 2022 Aug 31;13:1013711. doi: 10.3389/fimmu.2022.1013711. eCollection 2022. Front Immunol. 2022. PMID: 36119031 Free PMC article. No abstract available.
-
Transfused Red Blood Cell Characteristics and Kidney Transplant Outcomes Among Patients Receiving Early Posttransplant Transfusion.JAMA Netw Open. 2023 Sep 5;6(9):e2332821. doi: 10.1001/jamanetworkopen.2023.32821. JAMA Netw Open. 2023. PMID: 37707816 Free PMC article.
References
-
- Loubeau PR, Loubeau JM, Jantzen R. The economics of kidney transplantation versus hemodialysis. Prog Transplant. 2001;11(4):291–297. http://www.ncbi.nlm.nih.gov/pubmed/11871278. Accessed October 25, 2019. doi: 10.7182/prtr.11.4.n138851n77524hu1 - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

