Hospital readmissions and post-discharge all-cause mortality in COVID-19 recovered patients; A systematic review and meta-analysis
- PMID: 34781153
- PMCID: PMC8570797
- DOI: 10.1016/j.ajem.2021.10.059
Hospital readmissions and post-discharge all-cause mortality in COVID-19 recovered patients; A systematic review and meta-analysis
Abstract
Objective: The present study aimed to perform a systematic review and meta-analysis on the prevalence of one-year hospital readmissions and post-discharge all-cause mortality in recovered COVID-19 patients. Moreover, the country-level prevalence of the outcomes was investigated.
Methods: An extensive search was performed in Medline (PubMed), Embase, Scopus, and Web of Science databases until the end of August 3rd, 2021. A manual search was also performed in Google and Google Scholar search engines. Cohort and cross-sectional studies were included. Two independent reviewers screened the papers, collected data, and assessed the risk of bias and level of evidence. Any disagreement was resolved through discussion.
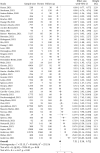
Results: 91 articles were included. 48 studies examined hospital readmissions; nine studies assessed post-discharge all-cause mortality, and 34 studies examined both outcomes. Analyses showed that the prevalence of hospital readmissions during the first 30 days, 90 days, and one-year post-discharge were 8.97% (95% CI: 7.44, 10.50), 9.79% (95% CI: 8.37, 11.24), and 10.34% (95% CI: 8.92, 11.77), respectively. The prevalence of post-discharge all-cause mortality during the 30 days, 90 days and one-year post-discharge was 7.87% (95% CI: 2.78, 12.96), 7.63% (95% CI: 4.73, 10.53) and 7.51% (95% CI, 5.30, 9.72), respectively. 30-day hospital readmissions and post-discharge mortality were 8.97% and 7.87%, respectively. The highest prevalence of hospital readmissions was observed in Germany (15.5%), Greece (15.5%), UK (13.5%), Netherlands (11.7%), China (10.8%), USA (10.0%) and Sweden (9.9%). In addition, the highest prevalence of post-discharge all-cause mortality belonged to Italy (12.7%), the UK (11.8%), and Iran (9.2%). Sensitivity analysis showed that the prevalence of one-year hospital readmissions and post-discharge all-cause mortality in high-quality studies were 10.38% and 4.00%, respectively.
Conclusion: 10.34% of recovered COVID-19 patients required hospital readmissions after discharge. Most cases of hospital readmissions and mortality appear to occur within 30 days after discharge. The one-year post-discharge all-cause mortality rate of COVID-19 patients is 7.87%, and the majority of patients' readmission and mortality happens within the first 30 days post-discharge. Therefore, a 30-day follow-up program and patient tracking system for discharged COVID-19 patients seems necessary.
Keywords: COVID-19; Hospital readmission; Mortality; Re-infection.
Copyright © 2021. Published by Elsevier Inc.
Conflict of interest statement
Declaration of Competing Interest There is no conflict of interest.
Figures


Similar articles
-
Association Between Dexamethasone Treatment After Hospital Discharge for Patients With COVID-19 Infection and Rates of Hospital Readmission and Mortality.JAMA Netw Open. 2022 Mar 1;5(3):e221455. doi: 10.1001/jamanetworkopen.2022.1455. JAMA Netw Open. 2022. PMID: 35258575 Free PMC article.
-
6-month mortality and readmissions of hospitalized COVID-19 patients: A nationwide cohort study of 8,679 patients in Germany.PLoS One. 2021 Aug 5;16(8):e0255427. doi: 10.1371/journal.pone.0255427. eCollection 2021. PLoS One. 2021. PMID: 34351975 Free PMC article.
-
Association of Hospital Discharge Against Medical Advice With Readmission and In-Hospital Mortality.JAMA Netw Open. 2020 Jun 1;3(6):e206009. doi: 10.1001/jamanetworkopen.2020.6009. JAMA Netw Open. 2020. PMID: 32525546 Free PMC article.
-
Hospital readmissions and emergency department re-presentation of COVID-19 patients: a systematic review.Rev Panam Salud Publica. 2022 Oct 10;46:e142. doi: 10.26633/RPSP.2022.142. eCollection 2022. Rev Panam Salud Publica. 2022. PMID: 36245904 Free PMC article. Review.
-
Effects of Transitional Care on Hospital Readmission and Mortality Rate in Subjects With COPD: A Systematic Review and Meta-Analysis.Respir Care. 2019 Sep;64(9):1146-1156. doi: 10.4187/respcare.06959. Respir Care. 2019. PMID: 31467155
Cited by
-
Target Trial Emulation Using Hospital-Based Observational Data: Demonstration and Application in COVID-19.Life (Basel). 2023 Mar 13;13(3):777. doi: 10.3390/life13030777. Life (Basel). 2023. PMID: 36983933 Free PMC article.
-
Healthcare utilization 9 months pre- and post- COVID-19 hospitalization among patients discharged alive.PLoS One. 2024 Jun 20;19(6):e0303509. doi: 10.1371/journal.pone.0303509. eCollection 2024. PLoS One. 2024. PMID: 38900737 Free PMC article.
-
Lessons Learned from Model-based Economic Evaluations of COVID-19 Drug Treatments Under Pandemic Circumstances: Results from a Systematic Review.Pharmacoeconomics. 2024 Jun;42(6):633-647. doi: 10.1007/s40273-024-01375-x. Epub 2024 May 10. Pharmacoeconomics. 2024. PMID: 38727991 Free PMC article.
-
Post-acute sequelae of COVID-19 among hospitalized patients in Estonia: Nationwide matched cohort study.PLoS One. 2022 Nov 23;17(11):e0278057. doi: 10.1371/journal.pone.0278057. eCollection 2022. PLoS One. 2022. PMID: 36417409 Free PMC article.
-
Treatment of patients hospitalized for COVID-19 with remdesivir is associated with lower likelihood of 30-day readmission: a retrospective observational study.J Comp Eff Res. 2024 Apr;13(4):e230131. doi: 10.57264/cer-2023-0131. Epub 2024 Feb 29. J Comp Eff Res. 2024. PMID: 38420658 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

