Correlations between preoperative diffusion tensor imaging and surgical outcome in patients with cervical spondylotic myelopathy
- PMID: 34786072
- PMCID: PMC8581918
Correlations between preoperative diffusion tensor imaging and surgical outcome in patients with cervical spondylotic myelopathy
Abstract
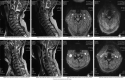
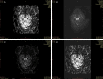
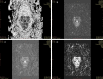
Objective: To investigate the correlations between preoperative diffusion tensor imaging (DTI), a Magnetic Resonance Imaging (MRI)-based technique and surgical outcome in patients with cervical spondylotic myelopathy (CSM).
Methods: A retrospective study of 95 patients with CSM who received diagnosis and surgical treatment in our hospital was carried out. According to the recovery rate of the Japanese Orthopaedic Association (JOA) scale at the 1-year postoperative follow-up, the patients were divided into a good recovery group (JOA recovery rate ≥60%, n = 47) and a poor recovery group (JOA recovery rate <60%, n = 48). Patients in both groups underwent diffusion tensor imaging examination before surgery. The preoperative fractional anisotropy (FA) value, apparent diffusion coefficient (ADC) value, longitudinal dispersion (AD) rate, and lateral dispersion (VD) rate were compared between the two groups. Pearson correlation coefficient was used to analyze the correlation between the preoperative DTI quantization parameters (FA, ADC, AD, VD) and the postoperative JOA recovery rate. In addition, we compared the preoperative spinal cord compression ratio (CR), spinal cord cross-sectional area (TA), maximum spinal cord compression (MSCC), and maximum canal compromise (MCC) between the above two groups. The correlations between the four measurements and the postoperative JOA recovery rate were analyzed using Pearson correlation coefficient.
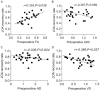
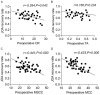
Results: The preoperative FA value in the good recovery group was significantly higher than that in the poor recovery group, while the ADC value was significantly lower (both P<0.001). The good recovery group had lower preoperative AD and VD, but there was no statistical significance (both P>0.05). Pearson correlation analysis showed that the preoperative FA value was positively correlated with the JOA recovery rate (P<0.05), while the VD value had significantly negative correlation with the JOA recovery rate (P<0.05). The preoperative ADC and AD values were negatively correlated with JOA recovery rate, whereas there was no statistical significance (both P>0.05). The CR, TA, MSCC and MCC values measured before surgery in the good recovery group were significantly lower than those in the poor recovery group (all P<0.001); were negatively correlated with the JOA recovery rate (all P<0.05), while the correlation with TA was not statistically significant (P>0.05).
Conclusion: DTI can evaluate the severity of the patient's condition before surgery by analyzing the subtle structural changes in patients with CSM. At the same time, the preoperative FA, VD, CR, MSCC, and MCC values are all associated with the surgery efficacy, which paves the way for the next step of clinical treatment.
Keywords: Diffusion tensor imaging; Japanese orthopaedic association recovery rate; cervical spondylotic myelopathy; correlation; fractional anisotropy.
AJTR Copyright © 2021.
Conflict of interest statement
None.
Figures
Similar articles
-
The Prediction of Neurological Prognosis for Cervical Spondylotic Myelopathy Using Diffusion Tensor Imaging.Neurospine. 2023 Mar;20(1):248-254. doi: 10.14245/ns.2244708.354. Epub 2023 Mar 31. Neurospine. 2023. PMID: 37016871 Free PMC article.
-
Feasibility of diffusion tensor imaging in cervical spondylotic myelopathy using MUSE sequence.Spine J. 2024 Aug;24(8):1352-1360. doi: 10.1016/j.spinee.2024.03.015. Epub 2024 Mar 29. Spine J. 2024. PMID: 38556218
-
Evaluation of DTI Parameter Ratios and Diffusion Tensor Tractography Grading in the Diagnosis and Prognosis Prediction of Cervical Spondylotic Myelopathy.Spine (Phila Pa 1976). 2017 Feb 15;42(4):E202-E210. doi: 10.1097/BRS.0000000000001784. Spine (Phila Pa 1976). 2017. PMID: 28207659
-
Magnetic resonance imaging assessment of degenerative cervical myelopathy: a review of structural changes and measurement techniques.Neurosurg Focus. 2016 Jun;40(6):E5. doi: 10.3171/2016.3.FOCUS1667. Neurosurg Focus. 2016. PMID: 27246488 Review.
-
Psychometric analysis and critical appraisal of the original, revised, and modified versions of the Japanese Orthopaedic Association score in the assessment of patients with cervical spondylotic myelopathy.Neurosurg Focus. 2016 Jun;40(6):E6. doi: 10.3171/2016.3.FOCUS1648. Neurosurg Focus. 2016. PMID: 27246489 Review.
Cited by
-
Comparison of the effectiveness of zero-profile device and plate cage construct in the treatment of one-level cervical disc degenerative disease combined with moderate to severe paraspinal muscle degeneration.Front Endocrinol (Lausanne). 2023 Dec 6;14:1283795. doi: 10.3389/fendo.2023.1283795. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 38125794 Free PMC article.
-
Evaluating tissue injury in cervical spondylotic myelopathy with spinal cord MRI: a systematic review.Eur Spine J. 2024 Jan;33(1):133-154. doi: 10.1007/s00586-023-07990-0. Epub 2023 Nov 5. Eur Spine J. 2024. PMID: 37926719
-
Correlation Between Pre-Operative Diffusion Tensor Imaging Indices and Post-Operative Outcome in Degenerative Cervical Myelopathy: A Systematic Review and Meta-Analysis.Global Spine J. 2024 Jul;14(6):1800-1817. doi: 10.1177/21925682231225634. Epub 2024 Jan 3. Global Spine J. 2024. PMID: 38168663 Free PMC article.
-
Negative Correlation Between Fractional Anisotropy on Diffusion Tensor Imaging and Neck Disability Index in Cervical Spondylotic Radiculopathy After Percutaneous Cervical Nucleoplasty: A Cross-Sectional Study.J Pain Res. 2025 Aug 8;18:3977-3986. doi: 10.2147/JPR.S530761. eCollection 2025. J Pain Res. 2025. PMID: 40799303 Free PMC article.
-
Biomechanical properties of a novel cervical spine implant with elastic deformation: a cadaveric study.Front Bioeng Biotechnol. 2023 Aug 29;11:1214877. doi: 10.3389/fbioe.2023.1214877. eCollection 2023. Front Bioeng Biotechnol. 2023. PMID: 37711451 Free PMC article.
References
-
- Badhiwala JH, Ahuja CS, Akbar MA, Witiw CD, Nassiri F, Furlan JC, Curt A, Wilson JR, Fehlings MG. Degenerative cervical myelopathy-update and future directions. Nat Rev Neurol. 2020;16:108–124. - PubMed
-
- Pehlivanoglu T, Wuertz-Kozak K, Heider F, Sauer D, Wanke-Jellinek L, Mayer M, Mehren C. Clinical and radiographic outcome of patients with cervical spondylotic myelopathy undergoing total disc replacement. Spine (Phila Pa 1976) 2019;44:1403–1411. - PubMed
-
- Maier IL, Hofer S, Joseph AA, Merboldt KD, Eggert E, Behme D, Schregel K, von der Brelie C, Rohde V, Koch J, Psychogios MN, Frahm J, Liman J, Bähr M. Quantification of spinal cord compression using T1 mapping in patients with cervical spinal canal stenosis-preliminary experience. Neuroimage Clin. 2019;21:101639. - PMC - PubMed
-
- Sun B, Shi C, Wu H, Xu Z, Lin W, Shen X, Wu XD, Zhang Y, Yuan W. Application of zero-profile spacer in the treatment of three-level cervical spondylotic myelopathy: 5-year follow-up results. Spine (Phila Pa 1976) 2020;45:504–511. - PubMed
-
- Zhang H, Guan L, Hai Y, Liu Y, Ding H, Chen X. Multi-shot echo-planar diffusion tensor imaging in cervical spondylotic myelopathy. Bone Joint J. 2020;102-B:1210–1218. - PubMed
LinkOut - more resources
Full Text Sources
